Prevention of Illness and Promotion of Health – not forgetting Cure
The four basic aims of the Charter for Health are:
- inform and educate everyone about health, so that they have the tools with which to press for better health.
- Provide organizational structures which facilitate rather than hinder the changes which an informed public will urge. To this end Community Health Councils will be strengthened and members of District Health Authorities will be directly elected.
- Minimum standards for all Health Authorities will be laid down by the Department of Health, and be monitored by a national inspectorate.
- A Cabinet Health Committee will be needed to ensure that every Department of Government is aware of the health aspects of its decisions. It will have the further responsibility to check that decisions by Departments at local level do not conflict in such a way that the health of individuals suffers.
Foreword by the President of the Socialist Health Association
This is a draft ‘Charter for Health’, and is a document for discussion.
We will welcome views and comments on matters raised in the pamphlet, and on the inevitable omissions relating to the policies a future Labour government should pursue in the interests of health promotion.
This draft is itself the result of widespread consultation over the last two years. It should be regarded as a preliminary document to be followed later by a further and more detailed publication.
While the election of a Labour government must be a first step towards better policies for health – especially the prevention of illness – such a government must have well worked out ‘healthy’ policies and strategies for all Departments from Cabinet downwards.
Please send individual and collective observations to us at 195 Walworth Road, London SE17 1RP.
Many members of the Socialist Health Association contributed to this Charter. I thank them all, and in particular Richard Stone, who wrote and re-wrote a mass of material into a coherent whole.
About the Charter
It will be seen that only one section of the Charter deals with the Department of Health. it is by far the longest because of the obvious need for reform within the NHS. However, there are other sections for almost every government Department, and this reflects how much the cause, care and cure of illness lie outside the NHS. Some sections are short. This is because they are intended to point to a way of looking at things rather than a compilation of detailed proposals.
Recommended reading
‘Inequalities in Health‘ (report of a research working group chaired by Sir Douglas Black) DHSS 1980
‘Fit for the Future’ (report of the Committee on Child Health Services chaired by Prof Donald Court) DHSS 1976
‘Prevention and Health – Everybody’s Business’ DHSS 1976
I Unemployment and Health in Familes’ by Leonard Fagin DHSS 1981
Royal Commission on the NHS. Cmnd 7615 1979
Introduction
The health of the nation will be best served by a major building programme and we can actually afford it because it will be self-financing. If anyone finds this is a surprising statement, they had better spend 50p on ‘What are the REAL causes of illness?’, the 25 page booklet from the Sheffield branch of the Socialist Health Association, available from the SHA, 195 Walworth Road, London SE17 1RP.
The cause of much illness is social and environmental, and beyond the scope of curative medicine. Specialists have known this for a long time, but only now is the understanding becoming more general. People become ill not just because nature visits illness upon them, but also because of the ways in which they live.
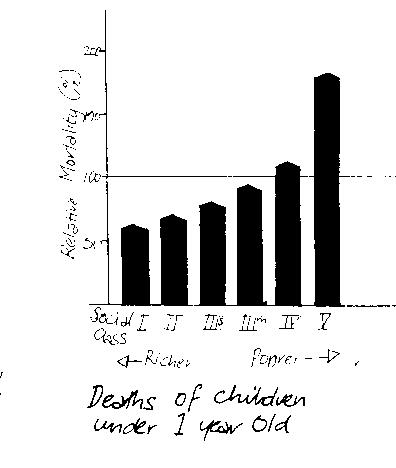
Ever since the Registrar General first published data by social class in 1911 it has been clear that illness and early death are more common lower down the socioeconomic scale. ‘Prevention and Health: Everybody’s business’, was published by the Labour Government in 1976. With the 1980 report ‘Inequalities in Health’ (the Black Report), it confirmed that, after 35 years of the NHS, the health of the nation as a whole has improved, but the gap in health between the rich and the poor has widened. The only possible conclusion is that, if manual workers and their families die younger and have worse health than professional people, then some of the extra deaths and some of the illness could have been prevented.
The Black Report found that it is inequalities in income, food, housing and working conditions which are the major influences in the inequalities in health. Concentrations of people suffering the effects of these inequalities are to be found in those inner city areas where the health and social services at community (primary care) level are at their worst. This ‘inverse care law‘ means that those most in need of a service are the least likely to receive it.
Health is truly at the root of socialism. Compassion for the suffering of the individual, and the desire to do something about it has always been a fundamental principle, but one which has rarely been at the front of political priorities in the British Labour Movement. ‘Health for All by the year 2000’ is the aim of the World Health Organisation. It is a worthy target for the Labour Party, which fits well with a commitment to spend on health rather than on buying nuclear bombs from the USA – or paying to defend 1,800 Falklanders as much as it costs the NHS for the health care of the 41 million people in Wales. Within the Health budget there will have to be choices on priorities in spending. The most urgent need was set out in the Black Report – a coordinated plan for ten ‘priority areas’ in the country which are the most deprived of primary care services.
The purpose of this Charter is to ensure that a future Labour government considers the policies of all its Departments in the light of their effects on the health needs of all sections of society. There is a growing realisation in the country of the way in which Tory policies ignore the physical and mental health of the majority of the people. Since the Falklands affair it has become a cliché to state that, where there is a political will, a government can do anything. This Charter for Health suggests ways in which, with the political will, any government can ‘get the economy going’. The economy would be led out of the recession by boosting domestic growth in the form of a massive building programme of homes, hospitals, health centres and schools. The economic growth would not have to be at the expense of health. This will answer the needs of people for decent homes, and so overcome the physical and mental ills that go with poor housing. The programme of building will also allow an expansion of the curative and caring parts of the NHS in many progressive ways which have so far remained only as pilot schemes – eg decent District General Hospitals linked to a network of community hospitals, health centres, residential homes and other facilities. The resulting increase in jobs and in living standards, especially for the less skilled who have been worst hit by high unemployment, would have an immediate effect on health. Furthermore, recent research confirms what is obvious from everyday experience: unemployment is associated with extra illness and early death, so the boost to the economy would reduce another of the major causes of illness. Large numbers of people would stop drawing unemployment and related benefits, and would start to pay income tax. At the same time the many secondary industries to building would increase their turnover, and so their taxes – haulage, brick companies, steel etc.
Government, management and unions all have an important contribution to make in promoting health. They need to be made aware of just how much they can do, if only so that anxieties about apparent cost, in taxes, in income and in jobs, can be overcome and turned to genuine desire to work together to improve all those factors, as well as the health of the nation.
Diversification of the tobacco industry, for example, is a vital preliminary to reducing cigarette smoking. Otherwise unions and management will understandably undermine any attack on their industry. Similar problems apply to reducing alcoholism. The problems of prevention of accidents relate to regulations and supervision in homes, factories and on the roads. All of these need considerable effort and coordination at grass roots and at high level.
Health Department
A. THE BACKGROUND
Prevention of illness and promotion of health are largely dependent on factors outside the health services. There is still an important role for the NHS and the DHSS. Despite much criticism, the NHS is held in high esteem, and appreciated by most people in the country.
The fundamental principles on which Labour based the NHS in 1948 were that the service is comprehensive for all citizens, free at the time of need, and paid for mainly out of general taxation. People when they are sick must not have the worry of whether they can afford fees, nor should professionals make a living only if they work for those who can pay.
There have been great improvements in the health of British people in the 35 years of the NHS. The average expectation of life has gone up from 62 to 70 years for men, and from 65 to 76 for women. Tuberculosis and polio have largely disappeared. Mortality rates for mothers and babies have tumbled down.
However, similar improvements in health have also taken place in other countries which do not have a National Health Service. Clearly then much of this has not been due just to the NHS.
1. What have been the benefits of our NHS?
1.1 We now have a national network of District General Hospitals – starved though they may be of funds. People do not now have to treck off to one of the old ,’voluntary’ hospitals to get a basic standard of medical and nursing care.
1.2 We have a system of primary care which is unique. Almost every person in the country is registered with a GP and one record envelope contains all medical details ‘from the cradle to the grave’. More than 90% of all consultations take place at this primary care level.
1.3 The system whereby referral to a specialist is by a GP, and specialists refuse (except in special circumstances) to see patients by self referral, safeguards patients against inadequate or bogus specialists – and therefore from exploitation. It also ensures that specialist skills are appropriately used.
1.4 Administrative costs of the NHS are well below those in comparable countries which have a pay and claim back system. In the USA and West Germany 20% of expenditure on health goes on administration. In the UK it is 5%.
2. What are the faults?
2.1 The presence alongside the NHS of a commercial system of health offers extra choice, but only to those who can afford it. It undermines the NHS, and anyone with a full time commitment to the NHS knows it. It encourages health professionals to adopt a market trader’s attitude, and takes consultants away from NHS patients. It takes away many of the most articulate patients who, if they were inside the system would be sure to insist that standards were kept high. It saps the morale of the dedicated people who work in the NHS. It destroys serious attempts at prevention of illness.
2.2 The GP, the pharmacist, the dentist and the optician remain independent contractors and have never been integrated into the local Health Authorities. New Tory legislation for Family Practitioner Committees strengthens this separation.
2.3 Only 20% of GPs work in Health Centres, and too many, especially in inner city areas, are single handed or in partnerships of only two doctors. There is no way in which primary health care teams can operate while the doctors are working like this.
2.4 Local people feel that they have little voice in the way that health care is organised. Community Health Councils are a very limited form of consumer representation.
2.5 Prevention of illness has been encouraged in policy documents from the DHSS, but little has been done. Critics talk of a National Sickness Service, rather than a National Health Service.
2.6 Until enough resources are provided for it, ‘Community Care’ will remain largely a slogan, coupled with exploitation of family willingness and support for sick relatives at home.
B. PRACTICAL PROPOSALS
1. Structure of the Health Services
1 .1 Private practice should be made unprofitable and discouraged. Full time service in the NHS should he positively and financially encouraged. Public subsidies should be abolished for what is, after all, a commercial enterprise no different from, say, the drug companies. This means that some commercial medical companies will lose their charitable status, and contributions to health insurance will not be allowed as a business expense.
1.2 Charges must be phased out. It is well known that the people who most need medical, dental and optical care are those least likely to get it. The deterrence of prescription charges and other charges must be abolished. The financial loss to the Exchequer will be small, since the costs of administration take up almost all the income anyway.
1.3 Democracy in the NHS is the only way to make local people know that it is their needs which are the first priority in local planning. The SHA plan is for:
i. District Health Authorities to have two thirds of their members elected by direct voting at the same time as municipal elections. The other third would be elected by the TUC affiliated trades unions in the local Health Service. Although the new kind of DHA will have wide powers, there will have to be a centrally controlled inspectorate to ensure maintenance of basic minimum care in all Health Districts.
ii. Regional Health Authorities. If elected Regional Government becomes a reality, then the RHA could well be a sub-committee of that elected body.
1.4 Family Practitioner Committees must be abolished so that community (primary) and hospital (secondary) planning can be integrated in one body, which will be the democratically elected District Health Authority. Independent contractor status should be replaced by a salaried service.
1.5 Community Health Councils will continue to have a positive role even after their matching DHAs have been democratically elected. To ensure that the voice of the consumer is heard, CHC effectiveness and funding will have to be, increased – as recommended by the Royal Commission on the NHS.
1.6 Health and Safety at work and Occupational Health need a national service to replace the sparse efforts made by employers so far.
- Finance for the service should, as now come from the employers, perhaps as a national levy. There would also have to be a major input from the NHS.
- District Health and Safety Committees would be set up as a duty by every DHA. Membership would include representatives of local trades unions, management and the DHA especially the health education department.
- Staffing of the service cannot be left to part time GPs. Training for doctors and technical staff (e.g. toxicologists) will be a high priority.
- Research into local accident risks and hazardous substances will be a duty of every committee. A wide definition of ‘hazardous’ is needed so that the less obvious damage to health (e.g. noise) is included in legislation. In addition the Dangerous Substances Regulations will have to be strengthened.
- Enforcement. The District Committee will have the power to monitor safety precautions by access for its staff to all work places in the District, including Crown property like hospitals, schools and old peoples homes which are at present exempt from Health and Safety Regulations.
- Occupational Health. The workplace should become a major centre of health activity. Monitoring of illness patterns will be extended from staff to include their families. Screening campaigns in the workplace can be linked by computer to screening in local health centres and GP surgeries to ensure that both working and non-working people in the District are all covered. Health Education at the workplace should be part of a wider expansion of health education to include pre-birth education in child care for men and women, pre-retirement advice and other needs as appropriate in the particular District.
2. Overall improvements in the Service
2.1 NHS staff
- Pay. Some NHS workers are among the lowest paid in the country. The Black Report showed that poverty is a major factor in high rates of illness and early death. By caring for the sick therefore, poorly paid NHS staff are themselves more prone to sickness. For this reason alone low pay must be abolished in the NHS.
- Levels of staffing should be high enough so that we no longer take advantage of the good will of ancillary and nursing staff, nor push junior doctors to work such long hours that mistakes are bound to be made.
- Financial inducements may be needed to encourage workers of all grades to work in unpopular parts of the country and in the less attractive areas of work e.g. long stay wards.
2.2 A hospital building programme is part of stimulating the economy and reducing unemployment. It will replace old hospitals with modern 700 – 800 bed District General Hospitals, and bring the rest up to date. Geriatric, psychiatric and GP beds will be needed in every District.
2.3 Minimum standards of care throughout the country set by, and monitored by the DHSS, have been a frequent request heard while collecting material for this Charter. Procedures and facilities have been developed in a few Districts which should by now have been made available everywhere. Examples are:
- laser treatment for eyes, and for abnormal cervical smears
- hip replacements done locally, and with short waiting lists
- stapedectomy operations for deafness
- locally based psychiatric services
- community psychiatric crisis intervention teams
- individual as well as group psychotherapy within the NHS
- abortion and sterilisation services.
This list is, and always will be endless. Information on new ways of doing things needs to be collected and evaluated centrally. At the appropriate time there must be the organisation ready to extend the new method to the whole country without delay.
2.4 Decisions on priorities. So long as demand for health care exceeds the supply of resources, there will be difficult choices to make on where to spend and where not. One of the advantages of having the District Health Authorities democratically elected is that these sorts of decisions can be made by local people who are properly accountable to an electorate. They should not be left to the lobbying power of consultants, or flag days, however worthy the cause.
2.5 Good statistics are important at primary level right up to DHSS. However figures are only worth collecting if they are going to be used for improving the way in which services are delivered.
A major review of the data collected by the Registrar General will have to emphasise, not just male occupation, which is an outdated arbiter, but more about the true social class of families and the geographical differences in health. Information should also be collected about factors which affect the dignity of patients – delays in transport, waits in out patient clinics, delays waiting for non-urgent operations, support for families with a dying relative and so on.
2.6 Research on health tends to be dominated by the drug companies – who are the ones who put up most of the money. It is not surprising that much of the work is about ways of curing illness with new drugs, especially for diseases which are widespread so that the profits from the research are likely to be high The DHSS should:
- set out a code of practice for a proportion of all drug company sponsored research to be concerned with prevention; and with the less common illnesses
- grant money itself, through its research organisations the MRC and the SSRC, for preventive work
- publish widely results of all work eve when, as with the Report on Inequalities in Health (the Black Report) it is politically sensitive.
i. Generic prescribing as proposed in the Greenfield Report, would reduce costs. It would also reduce unnecessary and potentially dangerous drug use.
ii. Drug companies. A major stake in the manufacturing industry is probably the only way to control the market force pressures which work against the needs of patients.
2.8 Choice within the NHS. People turn to the commercial medical companies because this seems to them the only way that they can exercise choice of where, and by whom they will be treated. Many assume that this is the only system for obtaining a second opinion. Even now these assumptions are not true.
- Choice of GP. The existing tentative steps by Community Health Council to inform people of the way to get off the list of one GP and register with another need to be expanded.
- Choice of consultant. Few patients a aware of that their GP can refer them to any consultant anywhere in the country.
- Second opinions. Most NHS consultants today are willing to give second opinions within the NHS.
- Alternative medicine. The beginning of alternatives to orthodox medicine are available on the NHS: some GP and Rheumatologists are learning osteopathic manipulations, and Homeopathy has always been available, though sparsely.
All of these elements of choice can, and should be expanded.
3. Primary Care
3.1 Salaried Service. To improve primary care we need to:
- unify community/hospital services
- increase preventive work
- attract practitioners to the less profitable areas, like remote villages and run down inner cities.
A major obstacle to all three is the self-employed status of GPs, dentists, pharmacists, opticians and chiropodists. A salaried service, as for hospital staff, must be the aim, with terms of service which answer the needs of all these professions.
3.2 Care in the Community is still little more than a slogan. Extra care means more staff: health visitors, community nurses (general and psychiatric) and midwives, all working closely with GPs in health centres. More home helps and meals on wheels will be needed, as well as transport and day centre provision. Development of the ‘family aid’, provided now by a few social service departments could give respite for caring relatives. More doctor time in the community can be achieved by reducing the size of lists per GP, and increasing the role of practice nurses as a part of the primary care team.
3.3 Health Centres. More than ever these are needed. Their existence will encourage formation of multidisciplinary teams serving their neighbourhood.
3.4 Dental Care. New ways to be tried out are:
- A capitation scheme for children, in the short term, during the negotiations towards a salaried service. This would be especially important in the ten priority areas suggested in the Black Report.
- Wider use of hygienists and other auxiliaries. This could be encouraged by granting to dentists the same 70% reimbursement for pay of ancillary staff allowed to family doctors.
- Community dental teams in all health districts with a brief to ensure that all sections of the community receive adequate dental care. Among the aims will be the elimination of inequalities that are geographical and tied to social class. Preventive dentistry would be made available to disadvantaged groups like the elderly and the handicapped.
- Universal fluoridation of water will need determined campaigns by the DHSS, followed by the necessary legislation.
3.5 Ophthalmic Service. Profit determines most of what patients receive. Better ways include:
- Proper fees to opticians for NHS work during the run up to a salaried service. This would allow them to concentrate on the prevention of blindness and partial sight without having to worry about making a living from promoting expensive frames.
- Design of frames needs to be modernised. They are still the same range as in 1948.
3.6 Chiropody is an essential service, which is grossly underprovided. It requires an intensive programme of reorganisation and expansion, including wider use of foot assistants.
3.7 Pharmacy is governed by profit from the producing drug company to the chemist’s shop. To change this into a service to patients will require:
- Proper fees to pharmacists in chemist’s shops, prior to a salaried service, so that they do not have to sell the medicines which are most profitable, as well as cosmetics, just to break even.
- Changes in the industry are set out above (2.6 and 2.7)
- Monitoring of drug effects by patients should be encouraged.
4. Prevention of illness
4.1 Self help groups are an important development in the democratic process. They also provide support for people with special needs, and so help to prevent illness. Health Authorities should give practical assistance when groups have been set up by local initiative.
4.2 DHSS as health watchdog. All health workers must be aware of every opportunity for health promotion, through an understanding of the harmful effects of unhealthy practices e.g. ‘junk’ foods, lead in petrol, unemployment, smoking, excessive drink, poor housing etc.
4.3 Health promotion teams should be set up by every Health District. Their annual reports would be reviewed not only by the DRA, but by the DHSS inspectorate to ensure that more than lip service is being paid to prevention.
4.4 Health Visitors are the only ‘outreach’ part of the NHS. They are ideally placed to bring the Service to those most in need of it, but, as the Black report showed, are the least likely to take it up. In particular:
- numbers of Health Visitors will have to be increased to allow small enough case loads for the extra work of going out to look for those in need
- attachment to GP group practices needs to be speeded up
- more motor cars are needed for health visitors to visit their patients.
4.5 Cigarette smoking has to be attacked:
- outside the Health Service – as discussed in the Introduction and the section on Environment (para 3)
- by making all hospitals no smoking areas
- by providing a counselling service in every Health District.
4.6 Screening programmes are best done in general practice, using a register of patients by Age and Sex. The register makes it possible to identify and contact people at risk e.g. the elderly, men liable to high blood pressure and women in the age range for pre-cancer of the cervix. The new DHAs, which will have Family Practitioner responsibilities, should be instructed to assist all GPs to set up Age/Sex registers, and to give encouragement and the necessary financial support to carry out these programmes.
4.7 Well people sessions. The list of categories is longer than most of us realise. Well Woman and Well Baby clinics are familiar, but there is a need also for Well Men, Well Elderly, Teenagers and People with Disablements. To these clinics, Health Districts should add Antenatal, Family planning, Sexually Transmitted Disease and Chiropody. The minimum number needed for each type can be calculated per head of population. The DHA should then ensure that there are the right number of sessions being held, preferably in Health centres or GP surgeries; failing which in separate clinics. Domiciliary services will be required to follow up non-attenders who often have the most need.
4.8 Child health – in the community as proposed in the Court report requires principally:
- developmental surveillance at key ages for all children by properly trained workers. These may be health visitors, family or clinic doctors.
- schools must be drawn in to these assessments. DHAs must work with Education authorities to make the school a focus for community activity.
- Encouraging closer family life is not mere sentimentality. The Court Report emphasised how essential for the proper development of each child it is to have a secure family. We must recognise that children can find that security in parental structures which are not just the traditional married mother plus father. Departments of Education, Health, Industry and Employment all have roles in encouraging men and women to lead a flexible enough life that they can be involved with their growing families.
4.9 Child health – in the school. The role of the School Health Service in health education of children requires further debate. The responsibility for teaching basic health education lies with the teachers, after appropriate training. This is discussed in the Charter in the section on Education and Science (para 5).
4.10 Child health – and child abuse. All families on child abuse registers should be offered intensive help to build constructive relationships in Family Day Units. Units at present do exist, run by the NSPCC or the occasional NHS psychotherapy centre, and these should be the models for all Health Districts.
4.11 Fertility control. Prevention of unwanted children leads to less stress in the parents, less mental breakdown in the family, less child abuse in the unwanted child and fewer disturbed adolescents growing up. Adequate services should be available equally in all parts of the country to allow people to control their fertility, and to choose when to have a baby. In many areas facilities for contraception are poor. Regional variations in NHS abortion services penalise women with less money who may be forced to continue with an unplanned pregnancy which a more wealthy person could pay to have terminated. Some women are not offered sterilisation when they ask for it, and then have to go through with a pregnancy which they do not wish to terminate, even though they may be at high risk due to age and many previous pregnancies DHAs must be required to provide adequate Family planning, Abortion and Sterilisation services.
4.12 Back pain is a huge contributor to distress and reduction of useful activity. Prevention involves education on how to avoid it. The Health and Safety at Work Acts could ensure that police, firemen, nurses, farmworkers and others are taught correct lifting techniques. Where furniture, car seats and so on are being made in local factories, Health Education Officers will need to be able to advise on design.
5. Topics for special emphasis
5.1 Health Education should
- be expanded into schools, the workplace, and other places where people meet e.g. centres and groups for the unemployed and residents’ associations.
- take on a wider role than simply telling people how to look after themselves. The more we are informed of the wav that uncontrolled commercialism and pollution damage health, the more pressure there will be for change.
5.2 Alcoholism. The task of diversifying the alcohol industry is dealt with in the section of the Charter for the Industry Department (para 1). Control of advertising of alcohol will be as for tobacco (Environment para 4). Treatment of alcohol addiction is the responsibility of every DHA, which should have diverse programmes offering a variety of treatments and goals. These would include programmes for the protection of workers and executives. Recovery programmes may or may not be run by doctors, but will require investment of capital. Attention must be paid to underlying provoking factors which create stress, like poor housing, poor education, and unemployment.
5.3 Ethnic minorities. In many cities there is an identifiable ethnic group who may have special health care needs e.g. thalassaemia, sickle cell disease, and of course language problems requiring an interpreter – not just any passing friend or hospital domestic, but a proper service. People may have special needs for intimate examination to be conducted according to the rules of their culture.
5.4 Women. Throughout this Charter policies are proposed many of which will improve the quality of life for women. The role of the media in portraying women as sex objects is dealt with in the section on the Environment (para 5). Education of children to question the stereotype of woman as housewife, and man as earner, is outlined in the section on Education (para 5).
In particular the DHSS can:
- set up special programmes to improve the health of women, to include not just the obvious medical schemes for cervical smears, family planning etc, but also promotion of women’s groups and other proposals suggested by local women themselves.
- encourage GP group practices to include a woman doctor.
- post notices at hospital appointment desks in all local languages notifying which of the doctors is a woman – there is usually one in most teams.
5.5 Childbirth. Many patients and staff have concerns about the Service.
- Patients want choice – to have or not to have the latest technology; to have the birth in a friendly hospital, or, with careful selection of cases and good back-up, at home. There is a positive role for obstetric staff in promoting mental health. They are well placed to identify families at risk of emotional stress during and after the birth, and to ensure that they are offered intensive support after returning home.
- Midwives are concerned that their role has been reduced. Only 20,% of the 100,000 trained midwives in this country are working in obstetrics and neonatal paediatrics, an average of one midwife for every 30 – 32 deliveries. More money needs to be put into the profession to increase salaries, combined with a radical revision of the work done to use their skills correctly and increase job satisfaction.
- GPs, properly trained, should be involved more in antenatal work as part of a team with the hospital. This is recommended by both the Royal Colleges of GPs and of Obstetricians.
- Obstetricians at consultant and junior level are too few to cope with the high level of emergency work, as well as with the new monitoring and screening procedures. Medical staff must still have time to talk with women. Each DHA will have to set up obstetric teams, with clearly defined roles for the GPs and hospital staff.
5.6 People with physical handicaps need more attention paid to their specific problems, in particular to the consequences of restricted mobility. More research will have to be promoted into the causes and control of pain, and more training for medical, nursing and paramedical staff in rehabilitation techniques.
5.7 Families of personnel in the Armed Forces are disadvantaged in ways which are not always obvious. They suffer from child/parent and husband/wife separations often with very little notice and for long spells. It is known that Child Abuse is reported four times as much in Forces families than in other families. The Armed Forces have their own medical services, separate from the NHS. Improvement of co-operation with the NHS and local social services for families, at least when they are in the UK, will have to be the subject of discussion. In particular, continuity of care must be properly organised to deal with the switch from barracks to civilian accommodation and back to barracks again.
Agriculture, Fisheries and Food
A. THE BACKGROUND
Agriculture and Fisheries occupy most of the time of this Department. As a result, the food industry has been able to sprawl at will in ways that are positively bad for the health of the people who eat what is produced. A large part of the cause of heart attacks, and other diseases too, is the diet which British people eat. Changes have been recommended by doctors and the DHSS, but little has happened. Reductions in consumption of sugar, butter and sausages, have been in the face of intensive resistance from the food industry.
The unchecked marketing of food results in all of us being pressed continuously to eat those foods which make profit, irrespective of their food value. It has been interesting to watch the response of the food industry to the message that fibre in food is good for us. The industry has responded by advertising those foods with bran in them as good for health, and sales have rocketed. It is ridiculous to see the Bran Flakes packet telling us how good it is for us because of its fibre content, with a box of Corn Flakes next to it, made by the same company, but with no mention anywhere on its box of the almost total absence of fibre.
B. PRACTICAL PROPOSALS
1. Information. The Ministry must take on a strong educational role in informing people about good and bad food so that they can make intelligent choices. Heart disease can be prevented by a diet of high fibre cereals and bread, with fresh vegetables and fruit, and less fatty meat products and dairy fat. Promotion of such a diet is an urgent necessity, and can only be achieved by a coordinated national policy.
2. Adequate and explicit labelling is needed to give us the chance to judge what we are buying.
3. A ‘Food Policy’ would be directed towards making healthy foods cheap and widely available. This would mean changes in agricultural policy, food manufacturing, food standards and marketing practises. In particular, subsidies would go on foods like wholemeal bread and low fat milk, instead of butter and sugar. Neither of these would in fact harm the farmers, but they and the manufacturers would need some short term help to change their processes in the minor ways required. The public sector is the nation’s largest cook. It could set a nutritional example by providing healthy food in schools, hospitals, military camps and government offices.
4. Reduction of sugar and salt in food processing and in products is required generally. This is especially important for those foods mainly eaten by children.
5. Food additives. Their harmful effects have become apparent in recent years and there are thousands of additives being used now. What is perhaps most alarming is the realisation that some children who have asthma, and some who are hyperactive, suffer from an allergy to the yellow colouring put in cakes, ice cream – and orange squash. Research is needed into this new field, but in the mean time additives should be banned unless they are needed for preservation, and not just to make foods look more attractive. Careful lists of additives are needed on all packets.
Cabinet
1. Health advice in the Cabinet is essential at all times in the formulation of Government policy. This would ensure that the health consequences of decisions are clear to Ministers. The Black Committee recommended “inter-departmental machinery in the Cabinet Office under a Cabinet sub-committee along the lines of that established under the Joint Approach to Social Policy.”
2. A Health Promoting Policy. It is at government level that strong guidance will have to come in shaping society in ways that answer the needs of people. People are becoming aware of how we have allowed our lives to drift into practices which damage our health. The recommendations of the Black Report are even more relevant now than in 1980 when they were first published. Their implementation is the change in direction which people increasingly want.
3. Impersonal bureaucracy must be avoided. The frustrations are not only irritating. They also result in those most in need of benefits and services being the least likely to receive them. Cabinet must give high priority to dealing with inconsistencies between actions of its members. It is no good looking after pensioners, for example, by DHSS increases in allowances which are then taxed away by the Treasury.
4. Structure of Government Departments. Some of the existing structures work against answering the needs of the worse off. The public in general, but in particular the elderly, the chronic sick and the poor might benefit from a unified service of health, personal social services, and housing. These sorts of options for coordinating and improving services should be examined.
5. Central/Local balance. Allowance for local initiative not only makes sense, but gives people control over their lives and thereby promotes mental health. Central directives should not be detailed orders; rather they should be in the form of strong directives which include minimum standards supervised by inspectorates. Detailed application should be by small flexible local units in which people affected by central decisions have democratic control. In this way central policy can be adapted to local needs.
6. Cigarette smoking. The Government must be seen by the public to be against cigarette smoking. There has to be a clear and determined policy that the tobacco industry will be prevented from damaging health. Education of the public will have to be coupled with help for the unions and the management to accept diversification of the industry. It may be that the only way to achieve this mammoth task is to take the whole industry into public ownership.
Defence
Nuclear Weapons
The ultimate in prevention of illness and premature death must surely be nuclear disarmament. In the words of the Quaker poster: “Let us take the risks of peace rather than the certainty of war”.
Working parties of the British Medical Association and of the Church of England have both produced reports (‘The Medical Consequences of Nuclear War’ and ‘The Church and the Bomb’) which show that any nuclear exchange will be total, and that there is no protection against the effects. Such an all out nuclear war will destroy civilisation, and threaten the very survival of our species. We fully support a non-nuclear defence strategy.
Education and Science
1. Health damaging school curriculums. A ‘healthy’ educational system is one in which individuals are able to develop their full potential in a non-competitive environment. The present system is geared too closely to the needs of the 6% who will go to University. This puts too much stress on the 6%, and condemns the other 94% to a permanent sense of inferiority. Education is more than academic subjects. It needs to prepare children for life as a whole.
2. Teacher: pupil ratios. It is almost impossible to vary educational methods to suit individuals when teachers are faced with 30 children at a time. Large classes are not only bad as a way of getting facts across, but they promote mental ill health in pupils – and in teachers. For the sake of the mental health of our future generations we must give children far more teachers.
3. Adult education is more than a luxury for promoting hobbies, important for mental health though hobbies are. It is also the means for people to change their career in mid life. Those who design adult education courses must realise the mental health promoting aspects of their work, and such openings should be readily available.
4. Under Fives. There is a need for education for children younger than five: it is important for their social and intellectual development. There is a beneficial effect on parents of sharing the care and knowing it is of the right type and quality for their child. To answer these needs of children and parents, a wide range of provision is needed e.g. full and part time nurseries, mother and toddler groups, as well as properly supervised child minders.
5. Involvement of parents in nurseries and schools must be promoted by all education authorities in order to overcome the distance between home and school environment. This will increase the closeness of family life and with it the mental health of the developing child.
6. Health education in schools
6.1 Compulsory for all children. Health education is not an academically inferior subject. Responsibility for teaching it lies squarely with teachers, all of whom should have completed in-service training before taking on this role.
6.2 The benefits of a healthy life style can be included somewhere in almost every subject -‘ exercise, diet, occupational health, safety at home and on the road.
6.3 Discussion of sexuality should encourage not only knowledge of the facts, but also responsibility in contraception. Preparation for parenthood begins at school. This time is an opportunity to help young people to be open about their feelings, not to have to hide sex, and to promote tolerance towards those who prefer not to fit into the stereotype of family.
6.4 Damage to health from drugs, cigarettes and excess alcohol is a topic easily avoided by teachers. In fact it needs to be spoken of often, and the teachers have to set an example by making even the staff room cigarette and alcohol free.
7. School Health Service and Primary Care were recommended to be integrated by the Court Report. This warrants further discussion and then implementation.
8. School meals should be free and available for all children. This is a major recommendation of the Court Report, which also proposed that parents would benefit from being involved in planning the content of their children’s meals.
9. Health Education of the Public needs more than the token nod it gets from governments. It warrants a whole Minister with a Department which will create public awareness of the possibilities for health. The benefits of increased public awareness are expanded in the Charter in the Health Department (Paras 1.3 and 5.1).
10. Fabric of school buildings will improve with the massive building programme proposed by this Charter as a way to improve health and stimulate the economy. In the short term, lead pipes in our many Victorian school buildings are one of the most potent sources of lead poisoning of children. They must be replaced quickly. Asbestos is too slowly being removed from schools.
11. Medical education
11.1 Prevention of illness and promotion of health need to be brought to a central place in the teaching of student doctors and nurses. Deans of medical schools and nursing tutors must be encouraged away from curing sickness as their main approach.
1 1.2 Recruitment of medical students is governed largely by high ‘A’ level results. This produces a bias towards pupils from academic fee paying schools, and from ambitious professional families. These students do not necessarily make the most caring and understanding doctors. New criteria for selection of future doctors are needed, and they should include encouragement of the ‘mature’ student, especially from among health service workers like laboratory technicians and nurses.
11.3 Training of community/GP and hospital doctors should include greater experience in each other’s field. The new GP training is doing this, but new hospital consultants would benefit from experience in general practice.
Employment
A. THE BACKGROUND
Even with the development of the microchip and subsequent technology there will never be a real shortage of paid activity for those able to work. What we have now is (a) some shortage of cash to pay people for it. (b) More important is the division of the work available which gives too much to some, ‘the employed’ and too little to the rest, ‘the unemployed’. Both groups suffer unnecessary illness as a result. There is an enormous amount of work which needs to be done in a civilised society which is not done at present. Our cities are far from clean. Roads and pavements are in need of repair. Home helps are too few.
B. PRACTICAL PROPOSALS
1. Unemployment
1.1 Reduction in levels must be sought for medical as well as moral and economic reasons. There are now several reports which confirm the increase of stress related disease in the individual concerned and in his or her family. What is not often realised is that physical illness has also been shown to be more common in the unemployed than in people in work of similar social class, background etc.
1.2 A massive building programme of homes and other socially useful buildings will ‘get the economy going’ and create new employment, especially of unskilled and semi-skilled jobs.
2. Employment
2.1 Management. Mindless work done by people who have no influence on their conditions at work not only leads to poor productivity and high turnover of staff; it is also known to increase mental stress with resulting mental and physical illness. Traditionally government does not interfere with management, either in the public or the private sector, but leadership must be given. People need to work in groups where they feel that they matter. They also need to be involved in decision making about their own work.
2.2 Flexible job structures. Policies should be devised which will encourage women and men to pursue their careers in work and in the family without detriment to either. Job sharing is the most familiar example. Work should be designed for people. We must stop bending people to fit the work.
2.3 Workers’ co-operatives do seem to achieve successful conditions of work in small industries. The Employment Department will have to find ways of applying this good practice widely in larger industries.
3. Parental leave
3.1 Maternity leave should be made flexible to allow for the differing needs of women and their employers. This could mean a choice of stopping work completely, or continuing part time.
3.2 Paternity leave is as necessary for the mental health of a family as is maternity leave. This was stressed in the Black Report: a secure family life is of prime importance to the normal development of every child. New legislation will be required for paternity leave to be a right.
4. A unified approach to the vocational training of young people needs to be developed. This would have to lead to permanent work on planned young workers’ schemes. The feeling of being rejected has to be avoided.
Energy
1. Nuclear fuel
It has become obvious from studies of nuclear power that the risks of danger to health from nuclear waste far outweigh any economic advantages. The lesson of the recent leaks from the Windscale (Sellafield) nuclear power station confirms the danger. In particular, installation here of American pressurised water reactors must be resisted. These are known to be favoured by the military as their choice for peaceful uses, because only this kind of power station can provide the right nuclear fuel for easy conversion to hydrogen bombs.
2. Lead in petrol
The dangers have been accepted by government, as are shown in the regulations to reduce lead. The time has come to abolish lead altogether.
3. Domestic Fuel Bills
We must eliminate once and for all self induced hypothermia through fear of high fuel bills. To ensure that everyone can afford heating in their home will mean:
i. Co-ordination of policy on pensions and grants for the elderly
ii. Controls on powers to cut off electricity and gas
iii. Strengthening the role of health visitors and other community workers in decisions about housing and social security payments for individual householders.
4. Minimum standards for homes
Safety and insulation must be brought up to higher standards, both in existing buildings as well as in the new.
Environment
1. Housing and Health
1. 1 A massive building programme of homes is a major proposal of this Charter.
i. Standards must not be at a low level just to save money. Ventilation, insulation and heating will have to be good, and energy saving and smoke control incorporated. Homes must be safe and large enough.
ii. Places to live in. These new homes must reflect the needs of the people who are going to live in them. The Byker housing scheme in Newcastle is a good model of a housing estate where the future inhabitants were involved in the planning, and the outcome has been a community with an environment which promotes mental health. This way new estates will have shops, play areas and other social facilities from the start.
1.2 Positive discrimination is required to provide healthy housing for disadvantaged people.
1.3 Single homeless. We must abolish hostels, and provide proper homes for single homeless people.
1.4 Categories of home must reflect changes in society. Single parent families are common. We have a much larger elderly population. Home building has to meet these changes.
1.5 Overcrowding. What few minimum legal standards are laid down for accommodation are often not applied. Many families live squashed into a single room with dangerous cooking and heating facilities, and often far too close to lavatories. Too many homes still do not even have internal lavatories. The legal definition of overcrowding must be updated from that which is still being used from the 1935 Housing Act, and very many more inspectors are required to enforce the laws.
1.6 Tenants’ Associations. Housing Departments should be instructed to promote tenants’ associations on all their estates, even those which are difficult to let. Where this has been done, the standard of living within the estate has always improved
2. Environmental Pollution
2.1 Lead in petrol, should be abandoned. (see Energy Department para 2)
2.2 Lead in water. The greatest source of lead which can get into children is in the water pipes of our many Victorian school buildings. The Environment Department should make available to Education Authorities the same grants that it does to householders to replace pipes. (see also Education Department para 10)
2.3 Radioactive and chemical waste. Very stringent controls of disposal are needed, and must be strictly enforced. This will need to be coupled to international regulations. We should not reprocess waste from other countries. This puts profit before safety and health.
2.4 Industrial pollution. Effluent into rivers and the sea, and gases into the air need to be carefully monitored, with particular attention to acid rain.
3. Cigarettes and Health
3.1 Advertising. Legislation is required to phase out advertising of tobacco products except at the place of purchase.
3.2 Sponsorship of sport and the arts by tobacco companies will have to be banned.
3.3 Diversification. Tobacco companies will be required to submit plans in consultation with their trades unions for the diversification of their products. The intention is the eventual phasing out of harmful tobacco products at home and abroad.
3.4 Health warning. A stronger, well presented health warning will have to appear on all cigarette packets and such advertising as remains.
3.5 Public non-smoking zones at first should be increased, leading to a change to non-smoking being the rule in public places, with designated areas for smokers.
4. Accident prevention
4.1 More one way traffic systems will reduce accidents because they reduce traffic flow in opposite directions. These half the relative speed at which vehicles hit each other, allow space for bicycle lanes, and allow greater distance between motor vehicles and pedestrians.
4.2 Child Accident Prevention Programmes are recommended in the Black Report for local authority planners, engineers and architects. Accidents are the main cause of death in children, the risk being seven times higher for working class than for children of professional classes. The programmes would be run by the local Health Education Department, with help from ROSPA. Special money will have to be given to local authorities, as well as to the Health Education Council.
4.3 Accidents in the elderly are too often the first step in loss of independence, institutionalisation, and the downhill slide towards death. Most accidents happen at home, and prevention therefore will have to start in the home where the health visitors are the best professionals for the job. This means increasing the numbers of health visitors, setting up Age/Sex registers and special training of health and social service staff in accident prevention. (see Health Department paras 4.3 and 4.5)
5. Advertising promotes sexism and racism
Attitudes are projected of:
i. women as sex objects
ii. men as tough and unfeeling
iii. people with coloured skin as not counting.
Tight regulations will have to be drafted which limit advertising and other distorting aspects of society. A body similar to the Press Council might be created to act as watchdog.
6. Health Care Strategy Committees
The SHA proposal (Health Department para 1.3) for Health Authorities to be democratically elected will have only a limited effect on Health Promotion. at a local level. Local Government is a provider of Education, Housing , Environmental and Social Services. It therefore has a major role as a ‘Health Authority’ in the widest sense. A Health Care Strategy Committee of the Council has been shown in Sheffield to be a very effective means of promoting health at a local level. Committees like this should be encouraged for all Councils. They would include all the members of the Council who have a health remit i.e. any members of the Council who are members also of Health Authorities or CHCs, with representatives of local groups in the health field.
Foreign and Commonwealth Office
The proposals in this Charter will improve the health and the economy of this country. By doing so there is a grave danger of exporting our ill health and poverty to less fortunate countries.
1. Health damaging substances may, as a result of proposals in this charter, no longer be sold in the UK. However, in order to keep up profits, Third World countries are already being found as an alternative outlet for cigarettes, powdered milk and expensive drugs not acceptable here. This exploitation of people in countries with even poorer controls than we have is not only immoral, but also damaging to the reputation of Great Britain abroad.
2. Unemployment will be tackled and reduced, but it cannot be truly overcome in isolation from the effects on other countries. Our Government will have to accept a role in other countries more than just promoting our trade at the expense of that of the rest of our ‘competitors’. We will have to work with countries rather than against them if there is to be an improvement in the health of people in other countries, for without that co-operation, our own efforts will come to nought.
Home Office
I. Mentally ill offenders. Many people in prison are mentally ill. Being sent to prison makes them worse rather than better. All prisoners should have a regular medical review with mental illness specifically looked for. This should be linked to a wide range of psychiatric and counselling provision.
2. The Prison Medical Service should be made part of the NHS. This would reduce the isolation of the staff, which in turn would encourage the caring and curing side of the work rather than mere custody. There might then be less of a tendency to prescribe drugs to subdue prisoners.
3. Sentencing policy now puts people in prison for many petty offences. This results in an excessively high prison population with overcrowding and over-use of drugs. The break-up of family life that also follows leads to misery and mental disturbance of the spouse and children. A policy of community work parole would be much better for the mental health of the offender and the family.
4. Policing. The recent trend back to community policing must be continued. This will create better relationships with the public who will feel confident that the streets are safer. This is particularly important for the elderly who must feel safe if they are to retain their independence.
5. Immigration Policy. Regulations which discriminate against women not born in the UK must be revised. They cause unnecessary stress and endorse racism.
Industry
A. THE BACKGROUND
Some industry is geared to production of goods which damage health. These industries will need help to change the goods they produce, accompanied by retraining of the workforce. Those concerned include makers of cigarettes, alcohol and nuclear weapons.
B. PRACTICAL PROPOSALS
1. Diversification of production away from health damaging goods means that companies will be required to submit plans in consultation with their trades unions for the diversification of their products. A good model of what will be needed is the plan put forward by the workers at Lucas Aerospace who produced a blueprint for ways in which they could use their specialist engineering and design skills on equipment for the disabled, rather than on weapons for killing thousands of people at a time.
2. Work environments. The ill effects of boredom and stress need to be understood by workers at all levels. They and managements can control, through their trades union and work place organisations the development of healthy working practices.
3. Health Education in the workplace. Expansion to take on a wider range of activity, and to include families of workers is proposed in the Charter in Health Department (paras 1.6 vi, and 5.1).
4. Known health hazards in the workplace are still killing and injuring people. The Employment Advisory Service must, as a matter of urgency, be handed over to the District Health and Safety Committees proposed by this Charter (Health para 1.6).
5. All reports of health inspectorates must be published. For example, the reports of the Alkali Inspectorates are never seen by the public, the press, and not even by. the workers whose health could be affected.
6. Industrial pollution is a problem of joint control by the Industry and Environment Departments, which should have an inspectorate responsible to both see Environment Department (para 2).
Social Security
1. Staff attitudes A change is needed throughout the DHSS to eradicate the tendency to regard Social Aid as a charitable gift, rather than the right of every citizen. It would help if staff were better paid, so that they are less likely to feel resentful of the amounts to which some claimants are entitled.
2. The Rules of Entitlement (the ‘A’ Code) need to be simplified. The Book must be published widely.
3. Child Poverty The Black Report considered “that the abolition of child poverty should be adopted as a national goal … this requires a redistribution of financial resources far beyond anything achieved by past programmes.” To abolish child poverty there will have to be increases on a generous scale in a wide range of benefits, including Child Benefits and Maternity Grants (see Treasury para 7).
Social Services
Variation in services from one part of the country to another is no longer an acceptable result of local democracy. It can be where need is greatest that social services are worst. Meals on Wheels and Home Helps may be cheap or free, and readily available in one borough, but expensive and sparse in another. Minimum standards are needed which are set centrally and monitored by a central inspectorate along the lines of the schools’ inspectorate.
Transport
1. Lead free petrol should be as much an aim of Transport as of the Energy and Health Departments. A coordinating committee from all three Departments will be needed to push through the necessary legislation.
2. A nationally integrated 24 hours a day transport policy with cheap fares would encourage the use of public transport. This would reduce road accidents. It would also reduce the stress associated with driving. There would be benefits to the economy from reduced costs of transport as well as of road maintenance. Many people are trapped at home by the inadequacies of public transport; town people cannot go out at night, and in the country there may be no means of getting from one village to the next.
3. Traffic systems. An increase in cycle lanes, wider pavements and one way traffic systems will save lives.
4. Reduced speeds limits (as in the USA) would reduce road traffic accidents. They would also result in conservation of large amounts of fuel. Limits must actually be enforced.
Treasury
1. The massive building plan proposed of homes and other socially useful buildings will benefit the Treasury in three ways:
- There will be a fall in payments of unemployment and other related benefits.
- There will be an increase in taxation coming in from building firms and their suppliers.
- Unemployed people will move from being a drain on the taxpayer to contributors of income tax.
2. Tax on health damaging goods. A huge increase in taxes on those commodities which are known to damage health would bring extra money to the Treasury. It would be a short term benefit, over 3-4 years perhaps, until the products were phased out altogether (see Environment para 3.3 and Industry para 1). Among the goods affected are cigarettes, alcohol and leaded petrol.
3. Bureaucracy. The Treasury must find ways of overcoming bureaucratic obstacles to cross-financing. ‘Care in the community’ proposed ways in which money could be transferred from Health to Social Services, but the difficulties are great and the resistance to such changes strong.
4. Private medicine. In order to promote the withering of the commercial health business, there should be no public subsidy by way of tax concessions on subscriptions to private health schemes.
5. Charitable status. Many private hospitals enjoy the benefits of charitable status, which bring considerable tax advantages. This flies in the face of their obvious commercial aims, which are no different from other businesses which touch on medicine, e.g. drug companies and medical equipment suppliers. Charitable status needs to be redefined.
6. Families with children. The tax and benefit system could be recast to redistribute resources to families when they are at the maximum stage of expenditure. Special efforts should be made to make constructive changes for one parent families.
6.1 Child Benefit. The first priority is to increase Child Benefit, making it index linked so that it improves in real terms as resources allow. In the longer term, child benefit should rise to the level of the Child Support Grant given to those on long term benefits.
6.2 Maternity Grant needs to be raised to a realistic level.
7. Death Grant has remained unchanged for 30 years. The hardship for some people-must be overcome by a generous increase.
8. Drug costs. Generic prescribing, and controls on the profits of the drug manufacturing industry (Health Department 2.6, 2.7 and 3.7) will save millions of pounds of tax payers’ money every year being paid out through the NHS.
THE SOCIALIST HEALTH ASSOCIATION CAMPAIGNS FOR:
A health service free at the time of use.
The abolition of all private practice within the NHS as an immediate objective and, in the longer term, the abolition of all private practice in this country.
Speedy democratisation of the NHS involving the dismantling of the Tory “managerial” structure.
The creation of an Occupational Health Service as an integral part of the NHS.
The nationalisation of the manufacturing, distributive and retail sections of the pharmaceutical industry.
A whole-time salaried service throughout all sections of the NHS.
More – and more comprehensive – health centres.
Re-orientation of the NHS to emphasise prevention and towards community-based services as opposed to a “hospital-dominated” service.
Greatly increased activity in the field of Health Education aimed at preventable illnesses and injury and in favour of positive health as opposed to mere absence of illness; creating systems by which patients are counselled and advised by all NHS personnel, particularly to reduce dependence on drugs.
Freely available advice and facilities throughout the country for birth control, abortion and sterilisation.
MEMBERSHIP OF THE SHA is open to every socialist who cares about the health of the people, whether employed in the NHS or not, and to all organisations in the Labour, Trade Union and Co-operative movements. We need the help of every socialist in the creation of a comprehensive, socialist health service.
CHARTER FOR HEALTH PUBLICATIONS:
1. “What are the REAL causes of illness?”
2. The Charter for Health
Both these pamphlets are available at 65p per single copy, or £5 for ten copies. Prices include postage and packing. Copies can be obtained from your local branch of the Socialist Health Association, or from national headquarters,195 Walworth Road, London SE17 1RP.
Printed by Leicester Printers Ltd Leicester & London (TU all depts) Second printing June 1984
