New Society 16 December 1976
Richard G. Wilkinson
As a Labour Secretary of State for Social Services you have the misfortune to be confronted by the largest social class differences in death rates since accurate figures were first collected in the 1920s and 1930s. Almost all the major causes of death including heart disease, stroke, lung cancer, stomach cancer, cervical cancer, pneumonia and bronchitis, are two or three times more common among unskilled manual workers and their families (social class V) than among senior professional and managerial families (social class I). Breast cancer is the only major cause of death which is more common among the upper classes than the lower. The overall death rate is now 50 per cent higher in social classes IV and V combined (the bottom quarter of the population) than it is in social classes I and II combined (the top quarter of the population).
No matter whether one looks at the relative or absolute size of the gap between the death rates of upper and lower social classes. it is two or three times as large now as it was in the early 1930s. It widened slightly during the 1930s and 1940s; it widened dramatically during the 1950s (in spite of the NHS): and it has continued to widen since then (see graph).
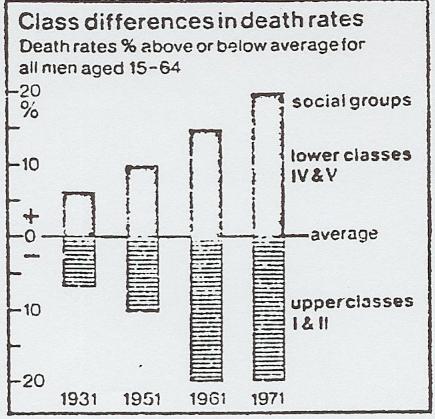
Of course you will want not only to halt this trend. hut also to reverse it. The widening gap in death rates tells us that people in bad conditions die younger than those in good ones. But it also shows that the higher death rates, even though they should be regarded as potentially preventable deaths, have fallen more slowly than the already lower death rates of the upper classes.
While a research student on a Health Education Council fellowship at the Department of Community Health, Nottingham University, I spent a year on a large-scale computer analysis of this problem and its possible causes. Other studies had already shown that, from the point of view of the overall death rate. what matters is not so much the standard of medical care for the sick, but whether or not you get heart disease, a stroke or some form of cancer in the first place. For this reason I confined my search for the causes of class differences in death rates to social and economic indicators related to class. Using figures from official sources, I looked at some 20 possible influences including housing conditions, overcrowding, jobs, education. air-pollution and so on as well as a number or social factors. Techniques of statistical analysis were used to compare these with death rates from 20 different diseases in the London and county boroughs. I then went on to look at the relationship between death rates and different items of personal consumption and expenditure in the regions of Britain.
My statistical results confirmed the findings of several other studies: factors such as housing conditions and occupational mortality now make little difference to overall death rate. They also confirmed the strong association between income and death rates, and showed that the relationship could not be explained away in terms of the indirect association of income with the other socio-economic variables I also looked at. The association between income and death rates seemed to be due almost wholly to the close statistical relationship between diet and death rates. The results were remarkably clear-cut and I should be glad to send you the statistical details.
Looking at the differences in diet between income groups it is not surprising that they have a dramatic effect on death rates. The following comparison lists the food consumption of households at the extreme, between the National Food Survey’s top and bottom income groups: The poor eat 56 per cent. less fruit per head than the rich, 19 per cent less fresh green vegetables, 28 per cent less cheese, 21 per cent less milk. 31 per cent less carcase meat, 8 per cent less fat. To make up for this the poor eat 57 per cent more potatoes, 33 per cent more cereal products (mainly bread), 32 per cent more sugar. “The rich” (income group A1) covers people who in 1974 were earning £5,000 a year or more. “The poor” (income group D1) covers those earning £1200 or less in 1974, but excludes old-age pensioners and households without income earners. Figures are eleven year averages, 1964-74 inclusive from the National Food Survey.
The only thing that is worse about the diet of the rich than the poor is the little bit of extra fat it contains. But the damaging effects of that are far out outweighed by the other differences between the diets. As a result, even heart disease is more common among the poor, despite the differences in fat consumption.
There seem to be six aspects of the difference between rich and poor diets which could lead to higher death rates among the poor.
First, people who are overweight tend to die younger and are particularly prone to heart disease, high blood pressure, stroke and diabetes. Many more of the poor are overweight than the rich. But this is not because they eat too many calories. It is because they eat the wrong ones. In recent years the diets of low income groups have contained an average of only 2 per cent more calories per head than the rich -in spite of their higher intake of potatoes. bread and sugar. These diets, disproportionately high in refined carbohydrates are also associated with some cancers.
Second, the poor eat. less fibre than the rich. This will not only cause higher rates of constipation. diverticular disease: and bowel cancer, but it has also been suggested that it contributes to heart disease, arteriosclerosis and possibly appendicitis.
Third, the rich get more of most vitamins than the poor. This will give them better resistance to most infectious diseases and could affect the early stages of some kinds of cancer.
Fourth, the higher sugar consumption of the poor would lead not only to increased tooth decay, but probably also increases risks of heart disease, arteriosclerosis and diabetes.
Fifth, there are a number of different theories stressing the importance to health of a sufficient amount of a variety of trace elements which are commonly found in fruit, vegetables, milk and meat. Most of these are much more plentiful in the diets of the rich.
Sixth, there is some evidence that several vitamins and lipotropic agents which occur in much larger quantities in upper class diets may play an anti-arteriosclerotic role, actually offsetting the artery-clogging effect of some of the rest of the diet.
None of these theories linking diet and disease are yet universally accepted by doctors and some are only accepted by a minority of medical research workers. But each one of them rests on a substantial body of corroborating evidence from both physiological and epidemiological sources. My argument does not, however, depend on any one of these still controversial theories, nor on the statistical results alone.
If diet is important one would expect sudden changes in the nation’s diet to produce changes in death rates. War-time food rationing radically altered the population’s diet. In particular, the first few years of the war saw a fall in the consumption of sugar and fat, and a rise in the consumption of fibre and probably also a rise in the consumption of vitamins. In response to these changes the civilian death rate fell – in spite of the worsening of housing and other environmental conditions, and the over-stretching of medical resources.
The end of food rationing also confirms the important influence of diet on death rates. The rationing system reached its height in 1947-48 and was dismantled between then and the early 1950s. Rationing had, as intended, ensured a high degree of equality of food consumption between different groups of the population. The current inequalities in diet arose while rationing was dismantled. The particularly dramatic widening of the gap between the death rates of rich and poor between 1951 and 1961 (again see graph) seems to be a reflection of the widening gap between their diets.
Looking at individual diseases, those which show the most dramatic shift in their social distribution during the 1950s are those which are already thought to have predominantly dietary causes. It was luring the 1950s that heart disease, which used to be a rich man’s disease, became a disease of the poor. It is likely that obesity also changed its social distribution during the war period. Diseases in which diet is a less important cause became rather more unevenly distributed than they were, but the shift was less dramatic than it was in heart disease.
To argue that diet is the key factor behind the trend in the overall death rate does not of course imply that it was the only, or even the main, cause of each disease. Most diseases involve a number of contributory causes. Smoking for example is firmly established as a main cause of lung cancer – explaining about 80 per cent of all deaths from lung cancer. But it is clear from statistics on smoking that the lower social classes are more prone to lung cancer per cigarette smoked than the higher social classes. At the most, then, diet could only play a minor role here. In heart disease on the other hand it seems to play the major role. Factors such as “stress,” which have been suggested as causes, are unable to account for the turn-round in the social distribution of the disease in the way that diet can. Such factors are likely then to play no more than minor underlying roles.
The prime importance of diet in the decline in the death rate since the last century has been shown by Professor Thomas McKeown and others. In a sense, my work just shows that their conclusions arc still valid in the 1970s. The only surprise is that diet is still important now that modern degenerative diseases and cancers have replaced the infections whose decline McKeown was mainly concerned with. It appears that, although we have developed a diet which gives us better protection against infections, we have needlessly linked the beneficial aspects with new, quite unrelated, damaging aspects such as the high consumption of fat, sugar and other refined carbohydrates, and a deficient consumption of fibre.
If I have managed to convince you that the nation’s diet is the most important single influence on the death rate, and that the differences in death rates between social classes are primarily the result of differences in diet, then what can the government, and you as Secretary of State for Social Services, do about it?
Clearly the NHS is not geared to undertake the kind of preventive work which is needed. Maybe an organisation such as the Health Education Council could play a part. At first glance the answer would seem to be to mount a campaign to persuade people to change their diets. But it would be wrong to expect that to make much difference. Such a campaign is likely to fail to do more than dent the problem because dietary patterns are determined more by income than by education.
There are several reasons for thinking this is so. First. statistical correlations show that diet is related more closely to income than education. Second, those people belonging to the middle and upper income groups who have large families to feed and clothe, tend to adopt dietary patterns more like smaller, lower income families. With additional children they may actually reduce their total family consumption of some expensive foodstuffs such as fruit. Third, while there is no significant difference between the number of calories consumed by high and low income groups, it is clear that the low income groups make up their total by buying more of the cheaper calories and less of the more expensive ones. The differences are not just chance differences in tastes.
The fact is, then, that the much higher death rates lower down the social scale reflect the fundamental inequalities in purchasing power in our society, While recognising that this problem is one of those demanding a radical solution, it would be wrong to ignore the effects which even minor changes in government policy can have on poverty and income inequalities. Policies on pay, on taxation, on the level of unemployment and on the exchange rate of the “green pound” must all have a direct impact on health. Indeed, the likelihood is that present policies are making the situation worse.
As Secretary of State, you will want not only to consider the broad strategy of economic policy in relation to health, but also the possibility of economic measures designed specifically to improve people’s diets. Food subsidies are however, problematic. If you subsidise foods such as fruit and fresh green vegetables which the poor should be eating more of, you are in effect subsidising the diet of the rich. Subsidise bread in the hope that the poor will have more money to spend on other foods, and you may find instead that still more bread is eaten.
To try to influence the food processing industries to change their products (or merely their recipes) is a possibility. Similar pressures have, after all, been brought to bear on cigarette manufacturers. Even a small decrease in the amount of sugar and saturated fat and an increase in the amount of fibre in processed foods would be an advantage. More attention should also be given to institutional meals, to school meals and to meals provided in factory canteens and old people’s homes.
If the government is to have, even moderate success in bringing down the death rates of the lower social classes – death rates which have not fallen significantly during the last quarter of a century – we know that health will need to become a major consideration across a wide area of food and agricultural policy where it has been conspicuously absent since the second world war. Unless effective action is taken we can only expect the differences in death rates and life expectancy between rich and poor to grow during your period in office as Secretary of State just as they did under your predecessors.
Dorothy Hollingsworth, the Director General of the British Nutrition Foundation, has emphasised the important influence which government policy and economic factors have had on recent trends in food consumption. She has also emphasised the lack of precise knowledge on how to influence consumption patterns in the desired direction. As a first step then, may I ask you to set up an urgent inquiry to look into these issues and to recommend action?
