Contribution to Health, Wealth and Poverty conference
Margaret Whitehead has covered a broad range of health determinants. I am going to concentrate on one. She has also mentioned eastern Europe, which to a considerable extent is an exception to what I have to say. I shall show the importance of income distribution – of relative income rather than absolute income – in most of the advanced OECD countries. The situation in eastern European countries is very different because there are still important absolute material factors affecting population health standards. Also income is not nearly such a good guide to status in eastern Europe. For example in a number of countries manual workers earn more than non-manual; also education and party membership have a much bigger influence on status. Margaret emphasised a concern for equity. What I want to do is to convince you that we should be interested in the social class differences in health not only from a concern for equity but as a recognition of the fact that they are a fundamental determinant of national standards of health. It is not simply a matter of social justice: if one wishes to improve the health standing of the whole population, equity is a key component -much more so than I had expected when I started this work.
Medicine and Behavioural Risk Factors
It is often assumed that we owe modern standards of health to the advance of medical science. But the decline in mortality from the great infectious diseases came long before medicine had identified their causes, or had any effective form of treatment or immunization for most of them. Other factors were responsible for their decline.
Although medicine has now become highly effective against many of the infectious diseases of the past, it has not yet gained a comparable power over most of the modern causes of death. If one looks at population measures of health – at death rates of the populations of developed countries, or their regions – it is very difficult to find any health outcome measures in the population as a whole which seem to be sensitive to variations in medical care, whether measured by expenditure, hospital beds or number of doctors per head of population. Even the death rates for just those diseases where medical treatment is highly effective are still more sensitive to variations in socio-economic standards than they are to differences in medical provision.(1) So, although medicine is good at hernias, varicose veins, cataracts and so on, it is not an important determinant of the population’s overall level of mortality.
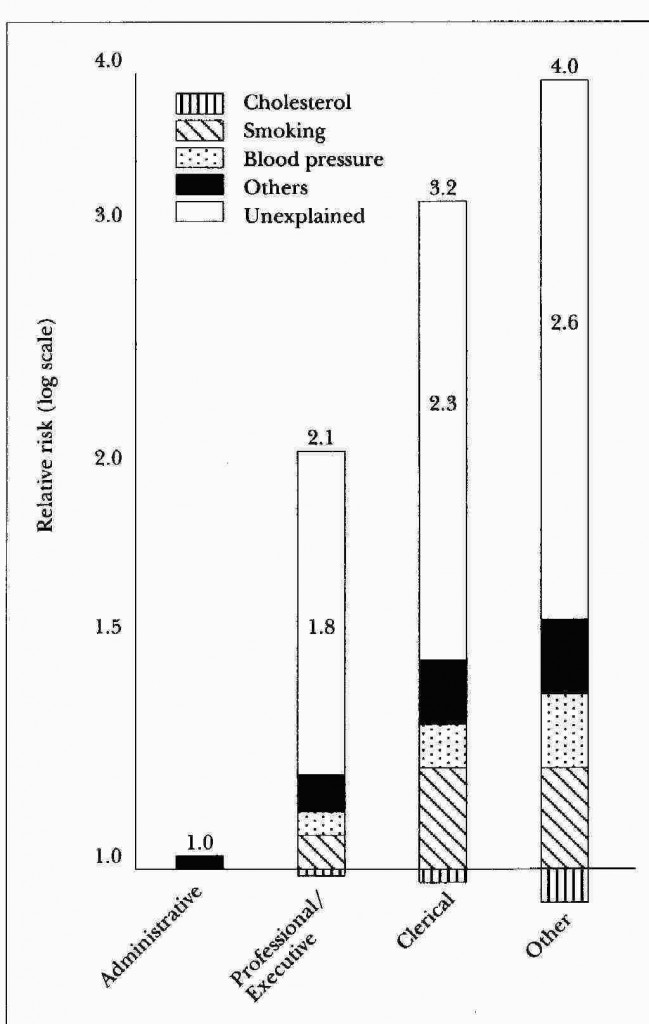
Figure 1 The relative risk of death from coronary heart disease among 17,000 civil servants working in Whitehall offices
| The bars show a 4-fold difference in risk between senior and junior workers. The shaded part shows the relatively small amount of the differences explained by the major known risk-factors. (“Others” include height, body mass, exercise and glucose tolerance.)Reproduced with kind permission from G. Rose and M. Marmot, Social class and coronary heart disease. British Heart Journal, 1981, 13-19. |
The other thing which is often assumed to be the over-riding determinant of health is personal behaviour – the do’s and don’ts of healthy living. Figure 1 is taken from the Whitehall study of 17,000 civil servants working in government offices in London. (2) It shows heart disease deaths for four ranks of office workers: administrators, executives, clerical and ‘other’. The death rate from heart disease is four times as high among the most junior as among the most senior staff. The shaded bands at the bottom of the columns in fig.l show how much of these difference can be explained by all the major known risk factors for heart disease. If instead we marked just the amount that behaviour can influence heart disease, probably less than a quarter of the differences would be explained. This is despite the fact that heart disease has been studied in more detail than almost any other single disease. It has been suggested that, even if you observe all the behavioural do’s and don’ts, your most likely cause of death is still heart disease.
Lung cancer is the only major cause of death for which known risk factors explain the bulk of the disease. Behaviour makes very much less difference to other causes of death where our ignorance of risk factors is so much greater.
Income Differences Within and Between Countries
The Black Report and the many studies of differences in morbidity and mortality amongst different social groups have reminded everyone of the crucial influence of socio-economic factors on health. Death rates are higher among the lower classes than the upper ones in 95% of the main causes of death in Britain.
You might then expect the overall standard of living to be an important determinant of national standards of health. Fig. 2 shows the relationship between GNP per capita and life expectancy (for men and women combined) among rich and poor countries. Among poorer, ‘third-world’ countries, life expectancy improves very quickly with increasing GNP per capita. However, among the rich, developed countries (in the horizontal part of the scatter in Fig. 2) there is little or no relationship. This is true not only when looked at on a cross-sectional basis: changes in life expectancy also seem unaffected by rates of economic growth. The correlation between them is almost non-existent.
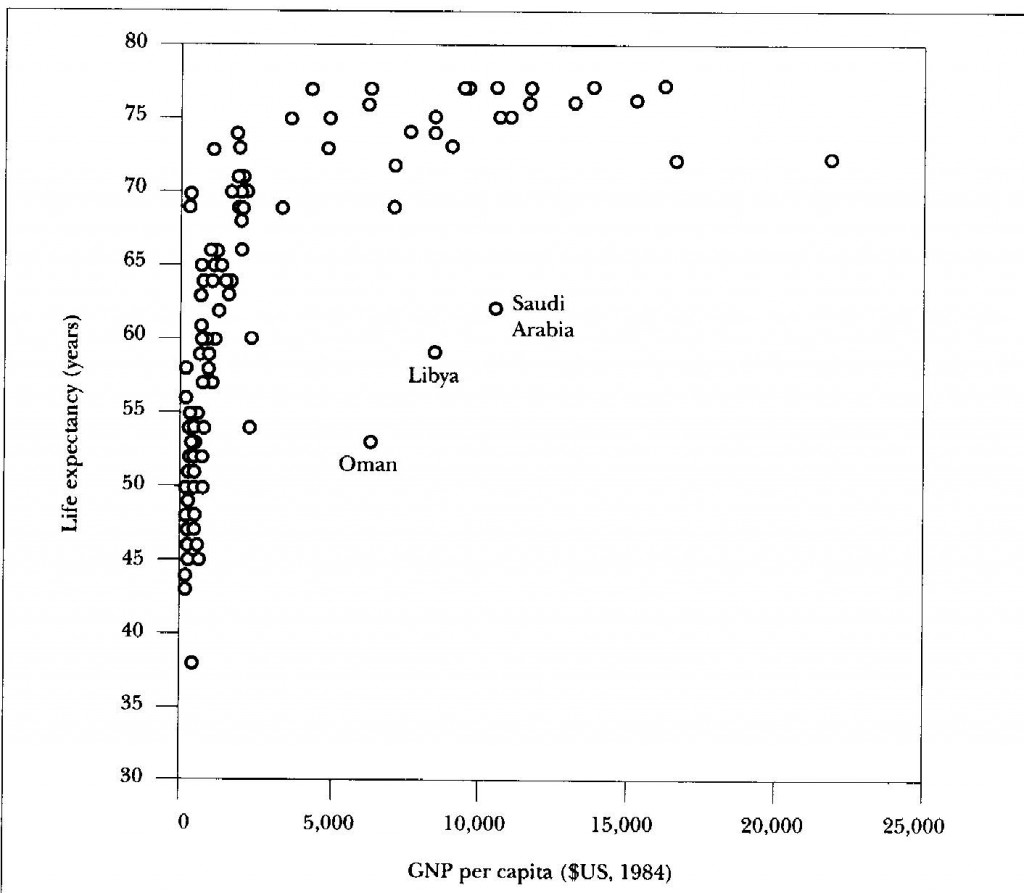
Figure 2 The relationship between Gross National Product per capita and life expectancy in rich and poor countries.
| Above a threshold level of income (here around $4,000) further increases in GNP per capita cease to have clear implications for longevity. The three outliers with life expectancy well below what might be expected from their GNP per capita are oil-rich states. Reproduced with kind permission from C. Marsh, Exploring the Data. Polity Press, 1988. |
This is a paradox. In the developed world, one country may be two or three times as rich as another without it making much difference to life expectancy. The result is the same if worked out using the real purchasing power of incomes in each country. The paradox is that although there is no more than a very weak link between the standard of living and life expectancy amongst the developed countries, if one looks within these same countries one finds a very strong relationship with the standard of living.
There is however a solution to this paradox. If health, or rather life expectancy, were related not to absolute income, but to relative income, then one would expect to find just -this pattern of a relationship within countries but not between them. Further, if relative income is important then one might expect to find a relationship between income distribution and life expectancy.
Income Distribution
I originally looked for a relationship between income distribution and mortality because I had found that the death rates of the less well-off seemed highly responsive to changes in income. It was Mildred Blaxter, an elder statesperson in this subject, who said she thought there was a relationship. It is very hard to find comparable measures of income distribution for different countries and the number of countries which can be included on any one basis is very restricted.
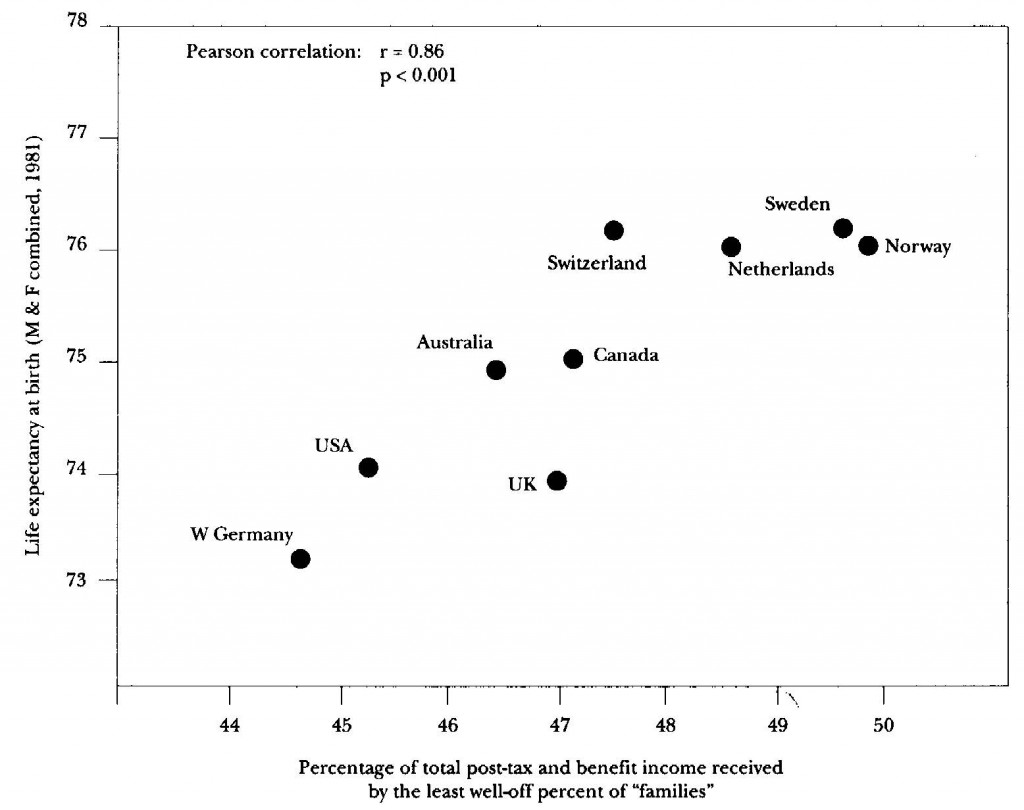
Figure3 The cross-sectional relationship between income distribution and life expectancy (M & F) at birth in developed countries c 1981
| Figure3 The cross-sectional relationship between income distribution and life expectancy (M & F) at birth in developed countries c 1981 |
| Data from JA Bishop, JP Formby and WJ Smith, International comparisons of income inequality. Luxembourg Income Study, 1989; Working paper 26 |
Fig. 3 shows the relationship between income distribution and life expectancy among one group of countries. Here Sweden, Nor way, the Netherlands have high life expectancy and more egalitarian income distributions; West Germany, USA, and the UK have less good mortality and are less egalitarian. Despite the very small number of cases this is statistically a highly significant relationship. It is such a much closer fit than I had expected to find that at first I thought it must be largely spurious and did little about it. It was only when reading that Japan now has the highest life expectancy in the world and the narrowest income distribution of any developed country that I started to see if changes in income distribution in different countries were related to changes in life expectancy.
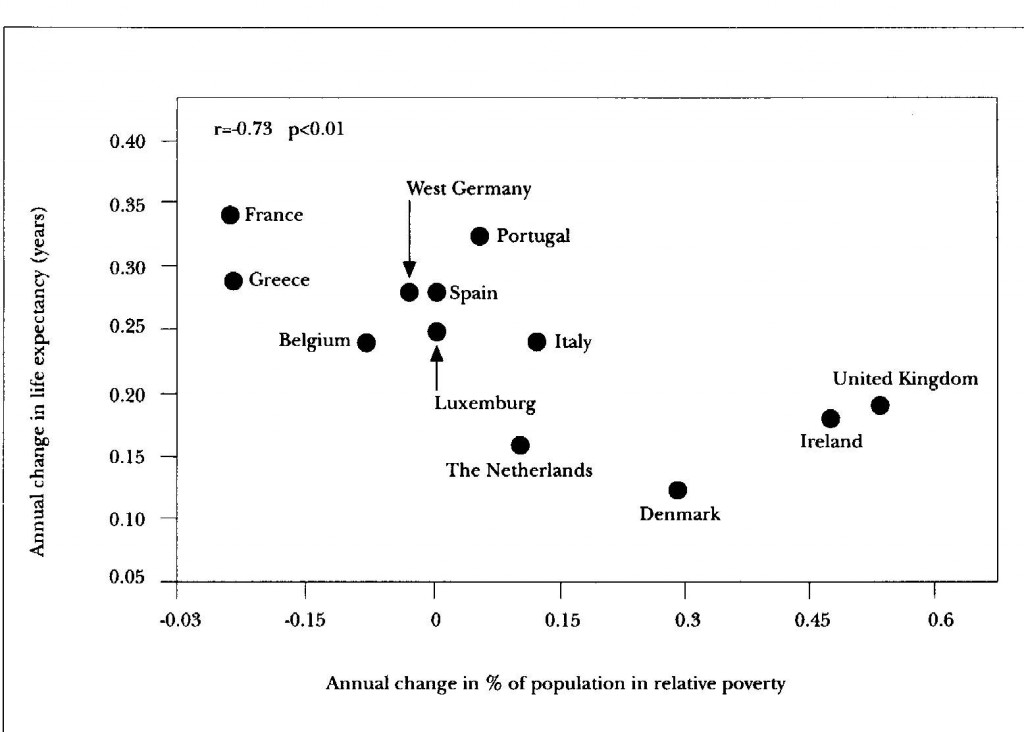
Figure 4 The annual rate of change of life expectancy in 12 European Community countries with the rate of change in the percentage of the population in relative poverty 1975-85
| Data from M. O’Higgins and S P Jenlins, Poverty in the EC in R.Teekens and BMS van Praag (eds.) Analysing poverty in the European Community, Luxembourg, EUROSTAT 1990 |
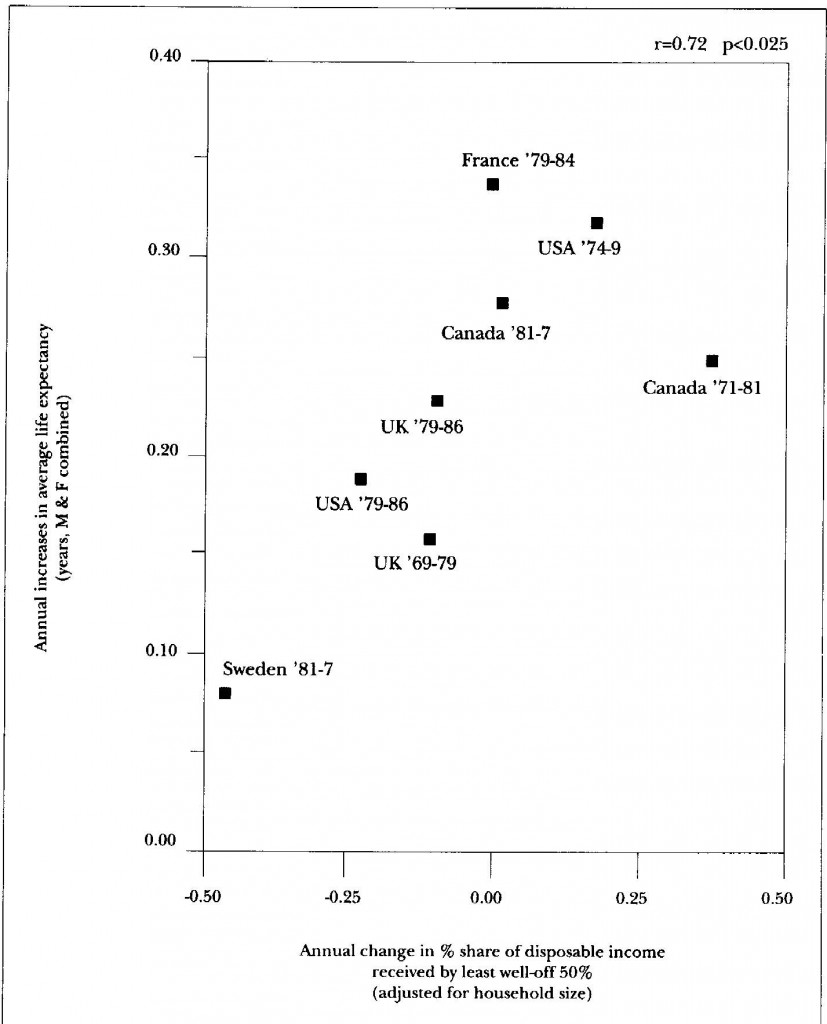
| Data from the Luxembourg Income Study |
Figs. 4 and 5 show what emerged. Both show annual rates of change in life expectancy plotted against annual rates of change in income distribution. Fig 4 slopes down rather than up like Figs. 3 and 5 because the horizontal axis shows increases in the proportion of the population living in relative poverty rather than the proportion of income received by the less well-off. Both show a statistically significant tendency for life expectancy to increase fastest where income distribution has narrowed and relative poverty decreased.
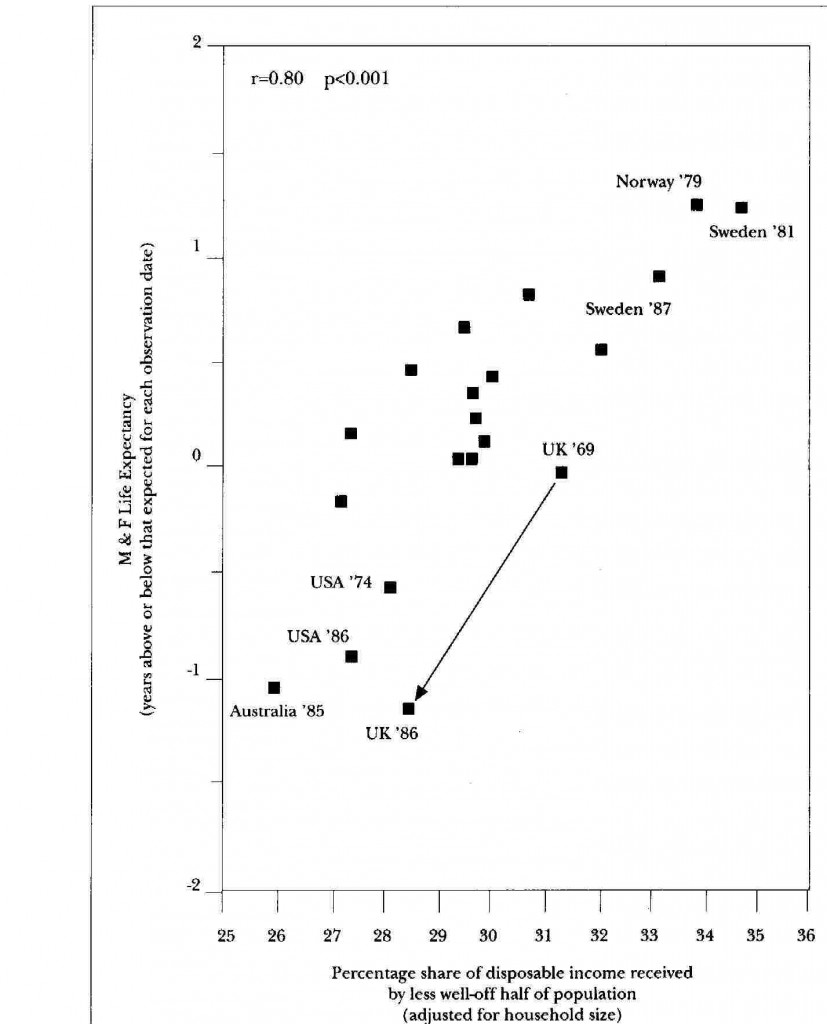
Figure 6 The relationship between income distribution and life expectancy adjusted for dates (excludes countries for which income distribution data excludes substantial minority populations.)
| Data from the Luxembourg Income Study |
Fig. 6 is slightly different. It is an attempt to combine all the comparable data from the Luxembourg Income Study despite the fact that income distribution was recorded at quite different dates. For some countries there are data for just one year, for others for several. The difficulty is that life expectancy tends to improve all the time (for reasons no one understands). To take account of this I controlled for the date of each observation. Thus the vertical axis shows whether life expectancy is above or below what is to be expected at the dates shown. Once again you can see a clear tendency for life expectancy to be better when income distribution is more egalitarian. It is particularly interesting to see that the relative slippage in the U.K’s life expectancy position (1969-86) is almost exactly what would be predicted from its widening income distribution. We can see that Sweden and the USA have also slipped relatively as their income distributions have widened.
These links between income distribution and life expectancy are confirmed by what little we know of what is happening to inequalities in health in different countries. For instance, while Japan’s income distribution has narrowed and its health has shot ahead, the health differences between blue and white collar workers have narrowed. Similarly, while Britain has declined relatively, the health differences between social classes have widened. In France, Britain and Sweden, where it has been possible to make very rough comparisons, it does look as if health inequalities are greatest where income differences are widest. Lastly, the evidence also suggests that changes in the proportion of people living in relative poverty in Britain has fed through to widen or narrow the social class differences in death rates.(3)
What appears to be happening then is that instead of health inequalities within each country representing health differences round a given average for that country, the position of the average is determined by the scale of the health disadvantage associated with relative deprivation in each country.
I have of course looked to see if this relationship could be the result of “reverse causality” – changes in health causing changes in income distribution – and there is little doubt that this can be ruled out. You might also think that the more egalitarian countries would also have better public services which might lead to the association with better health. Not only are relationships such as these an implausible source of a relationship as close as that shown in Figs. 3-6, but I have also found that controlling for various areas of public expenditure does not explain the relationship.
The next point I want to make concerns the size of the effect. It is too large to explain in terms of changes in the health of small minorities of the population alone. You would not produce this size of effect on overall mortality even if you cancelled out the whole of the health disadvantage of Social Classes IV and V. The effect is more widespread than that. If you look at the pattern of correlations between different deciles of the income distribution, you find that it is the income share going to the whole of the bottom half of the population that seems to be most closely related to the population’s average life expectancy.(4)
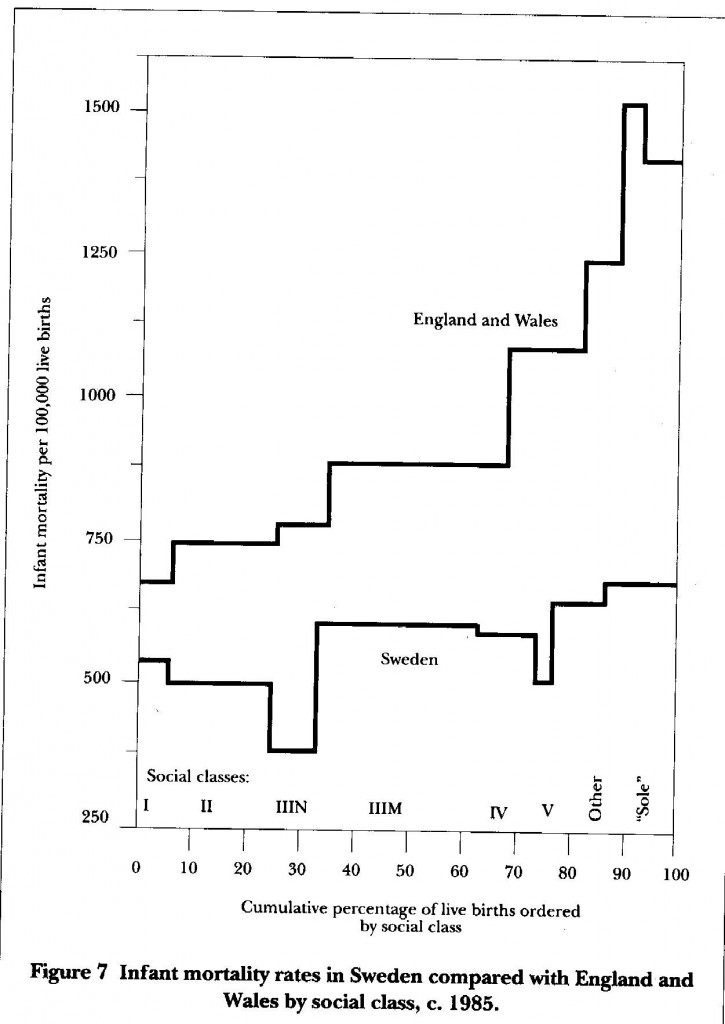
| The width of the “steps” is proportional to the percentage of live births in each social class. “sole” =Births registered in mothers name only |
| Data from D. Leon, D. Vagero and Otterblad Olausson, Social class differences in infant mortality |
Another thing that indicates the possible scale of this effect is the contrasting pattern of social class differences in death rates in Britain and Sweden. The comparisons are soundly based because researchers in Sweden have actually used the British Registrar General’s social classification to classify their deaths. The differences for infant mortality are shown in Fig 7. In Sweden, where income distribution is so much more egalitarian than in Britain, the gradient of infant mortality with social class is shallow and inconsistent. Even more important is that the highest death rates in Sweden are similar to the lowest in Britain.
This is not hard to understand; indeed there are good reasons why income distribution affects mortality even in Social Class I. Relative poverty is not wholly confined to the lowest social classes. Because the fit between income and occupational class is not good, social class I includes some of the poor. Unemployed solicitors are still classified as Social Class I and there will also be directors of small companies losing their houses because of not being able to keep up with the mortgage payments in a recession. This means that increases in relative poverty can raise death rates in all social classes -though obviously the effects will be greatest as the proportion of those on low incomes increases lower down the social scale.
The same pattern can be seen in the adult mortality rates in Sweden and Britain. Mortality among people of working age in the Swedish lower classes is at least as low as in Britain’s upper classes.(5)
Psychosocial Links
What does all this add up to? What it tells us about society may be even more important than what it tells us about health. The evidence that we are dealing with the effect of relative rather than absolute income, particularly the lack of a clear relationship with the absolute standard of living as measured by GNP per capita, points to the importance of psychosocial over material influences on health. If we were dealing with the direct physical impact of people’s exposure to poorer conditions, then other people’s standard of living would not matter. Quite contrary to the evidence we have seen, the absolute standard of living and economic growth would solve all the problems. Relative income implies that cognitive, comparative processes are involved.
It is quite hard to think how relative income can be important unless it is through psychosocial channels. It suggests that the main impact is not directly a matter of your circumstances themselves but is related to what you feel in them. This is not to say that damp housing does not affect your health – it does. People have identified quite accurately, with good methods, that there are excess respiratory diseases among people who live in damp housing which can be related to the presence of mould spores in the air. (6) But that accounts for only a very small part of the excess illness and deaths amongst people in poor housing. The rest of it has to be explained by what being in that kind of inferior housing, in those social circumstances, does to your sense of yourself and your subjective quality of life. What matters is the depression, isolation, insecurity and anxiety caused by low incomes.
Some of the work on unemployment and health confirms the importance of these psychosocial links. When a food processing factory closed in Calne in Wiltshire, GP records showed that illness (including hospital referrals for serious conditions) went up immediately redundancies were announced – some time before people actually became unemployed. (7) This shows that the sense of insecurity and worry is central to the causal process. There is now a good deal of epidemiological evidence, often backed up by animal studies, demonstrating the importance of a number of psychosocial factors in health.
Percentage of people in income groups in households with various consumer durables
| Income group: | Poorest 20% | Poorest 50% | Total popn. |
| Freezer | 68 | 76 | 83 |
| Fridge | 97 | 98 | 99 |
| Television | 98 | 99 | 99 |
| Telephone | 68 | 78 | 87 |
| Car or van | 42 | 54 | 69 |
| Washing machine | 80 | 87 | 90 |
| Central heating | 69 | 72 | 79 |
| Video-recorder | 47 | 53 | 63 |
From: DSS, Households below average income 1988/9. HMSO 1992.
In this discussion it is important to have a clear idea of what relative poverty involves in Britain today. The table shows some of the official figures of the ownership of different consumer durables in various income groups. They show that even among the poorest 20 percent of the population, a large majority have a freezer, a fridge, T.V., telephone, washing machine and central heating, and almost half have a video and access to a car. Obviously these consumer durables will be very different from those of the rich.
It may be that increasingly in our society this is the basic equipment that everyone needs in order to get along. Part of the problem is no doubt the stress caused by the £90 bill when a washing machine pump packs up or you get caught with inadequate tread on car tyres you cannot afford to replace. These are financial disasters for people on low incomes. Financial stress has been shown to be one of the main sources of anxiety and of marital failure.
People sometimes suggested that it is a cop-out to interpret this relationship between income and health as a matter of psycho-social factors. I disagree. Suppose it was all a matter of poorer nutrition in lower social classes. First you would expect that to be dealt with by economic growth over a period of a decade or so. You would also have expected that class differences in health would have narrowed instead of widened with the rising absolute level of affluence in the post-war period. But the point is that poorer nutrition would have a less fundamental effect on people’s subjective quality of life than the psychosocial factors that permeate one’s whole consciousness. Eating a cheap diet may be less healthy, but in terms of the quality of life the difference in taste is nothing compared with the depression, anxiety, sense of failure, insecurity, loss of self-esteem, poor social relations and worry caused by inadequate incomes. Those feelings can reduce the subjective quality of life to nil – as the association with suicide testifies.
These social implications of income distribution will stay with us whatever standard of living economic growth may get us to. They have to be tackled head on by narrowing income differences. Even for those affected it is not necessarily the health effects of their income position which they would mind most. It is the more immediate difficulties, worries and insecurity that people face when trying to cope on small incomes which matter.
Another objection to accepting a psycho-social interpretation of this relationship is the belief that psycho-social factors are individualistic and lead only to psychotherapy as a solution. But the point about relating psychosocial factors to income distribution is precisely that it shows there are structural factors which do affect the psychosocial quality of the population’s life. More than that, it is amenable to policy. Governments cannot help but affect income distribution. It is the extremes of income – the rich affected so fundamentally by tax levels and the poor by benefits – which mean that government policy is inevitably influential. The last point is that if my interpretation of this data is correct then one would also expect these income differences to haveother fundamental effects on the social fabric. There is some evidence of an effect on children’s educational performance, on levels of crime and no doubt on other aspects of social life. We are only beginning to be able to look at things like this as internationally comparable measures become available. It may well be that income distribution has a fundamental effect on the quality of the whole social fabric of a society.
References
1. MackenbachJP, Bouvier-Colle MH, Jougla E. Avoidable mortality and health services: a review of aggregate studies. Journal of Epidemiology and Community Health. 1990; 44: 106-11
2. Rose G, Marmot M. Social class and coronary heart disease. British Heart Journal 1981; 13-19.
3. Wilkinson RG. Class mortality differentials, income distribution and trends in poverty 1921-81. Journal of Social Policy 1989; 18 (3): 307-35.
4. Wilkinson RG. Income distribution and life expectancy. British Medical Journal 1992; 304: 165-8.
5. Vagero D. and Lundberg O. Health inequalities in Britain and Sweden. Lancet, 1989; ii: 35-6.
6. Platt SD, Martin CJ, Hunt SM, Lewis CW. Damp housing, mould growth and symptomatic health state. British Medical Journal 1989; 2 98: 1673-8.
7. Beale N, Nethercott S. The nature of unemployment morbidity 2. Description. Journal of the Royal College of General Practitioners 1988; 38: 200-2.
