by Ted Schrecker and Clare Bambra
Within the small local authority of Stockton-on-Tees in the North East of England (population 192,000), the difference in male life expectancy between the most and least deprived areas is 17 years – comparable to the difference in average male life expectancy between the UK and Russia or Senegal. In Washington, DC around the turn of the century, the difference in male life expectancy between the poor (and predominantly black) southeast of the city and the wealthy, overwhelmingly white suburbs in Maryland was even larger (20 years).
These health inequalities reflect underlying social and economic inequalities. Since the early 1980s, neoliberalism or “market fundamentalism” has dominated discussions about politics and economics across much of the globe. In our book Neoliberal Epidemics: How Politics Makes Us Sick we consider the health effects of over three decades of these policies with particular reference to the US and the UK. We identify four neoliberal epidemics: austerity, obesity, stress, and inequality. They are neoliberal because they are associated with or exacerbated by the rise of neoliberal politics. They are epidemics because they are on such an international scale and have been transmitted so quickly across time and space that if they were a biological contagion they would be seen as of epidemic proportions.
Addressing the 2014 annual joint meeting of the World Bank and the International Monetary Fund, the Fund’s managing director Christine Lagarde described the growth in inequality worldwide as “staggering”. Its dimensions in the US and the UK certainly merit that description, largely due to increases in the income and wealth share of the top 1%. In 2014, it was reported that the combined wealth of the 104 richest individuals living in the UK amounted to more than £301 billion, and that the wealth of the UK’s five richest families alone exceeded the net worth of the bottom 20 percent of the population. In the US, the share of the nation’s wealth of the top 0.1 per cent (one one-thousandth) of the population increased from 7 percent in 1978 to 22 percent in 2012 – comparable to the inequality of distribution before the Great Depression, and roughly equal to the net worth of the bottom 90 percent of the population, which had fallen from 35 per cent in the mid-1980s to 23 percent.
This trend partly reflects growing inequalities in market incomes (wages, salaries, bankers’ bonuses, stock options and investment income). However in the UK and especially in the US, the growth in the income share of the top 1% that began circa 1980 is also a result of sizable reductions in the marginal income tax rate for top earners. The main beneficiaries were the richest 1% of the population. In the UK, the Gini coefficient – a key measure of income inequality – rose rapidly throughout the neoliberal Thatcher era, and has not fallen substantially since then. Perhaps not surprisingly, on some measures health inequalities between the richest and poorest local authority districts in England were larger than at any point since before the Great Depression even before the financial crisis. And while most people are only just recovering from the effects of the 2008 financial crisis, or are falling farther behind, the wealth of Britain’s richest thousand families has doubled.
In The Spirit Level, epidemiologists Richard Wilkinson and Kate Pickett concluded that high levels of inequality have negative health effects throughout entire societies, although multiple causal pathways are involved. For example, life expectancy and infant mortality are correlated with the level of income inequality across high-income countries and, within the US, across states. Five years after their book was published, the evidence appears even stronger. Meanwhile, the deepening economic inequality promoted by neoliberal societies has greatly reduced social mobility so that your parents’ income, job and education now determines your own future social position and health to a greater degree than at any point since the second world war, at least in the UK and the US where social mobility has declined since 1980.
Today’s high levels of inequality in countries that have travelled the neoliberal road are the result of political choices – choices that could have been made differently. Geographer Danny Dorling points out that similar trends have not occurred in many other high-income countries, such as the Scandinavian countries with social democratic welfare regimes. “Only some rich countries recently set out to become more unequal”. And the illustration shows that in high-income countries the proportion of people living in poverty, on a measure designed for such cross-national comparison, varies threefold. This is not a reflection of differences in market incomes, but rather of political choices about how the product of a society’s economy, and its accumulated wealth, should be distributed. Rather than being a fact of economic or political life, inequality is a neoliberal epidemic: one of the ways politics makes us sick.
Poverty rates before and after taxes and transfers, selected OECD countries,
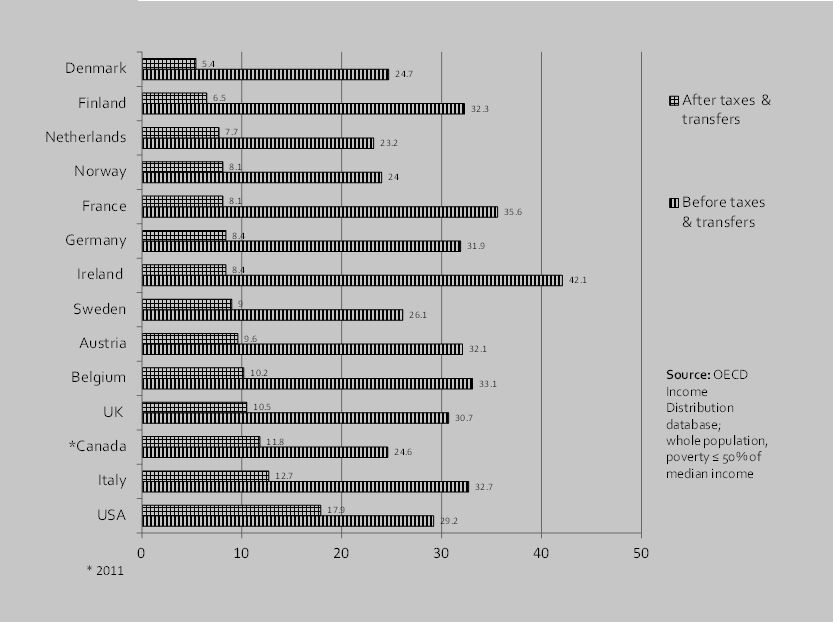
2012 (except as noted)
Links: Schrecker, T. and Bambra, C. (2015) Neoliberal Epidemics: How Politics Makes Us Sick, Palgrave Macmillan, available at: http://www.palgrave.com/page/detail/how-politics-makes-us-sick-ted-schrecker/?K=9781137463098
About the authors
In June 2013, Ted Schrecker moved from Canada to take up a position as Professor of Global Health Policy, Centre for Public Policy and Health, Durham University (UK). Since 2002, most of his research has focused on the implications of globalization for health; he also has long-standing interest in issues at the interface of science, ethics, law and public policy. A political scientist by background, Ted worked as a legislative researcher and consultant for many years before coming to the academic world, and co-edits the Journal of Public Health. Among his publications, he is editor of the Ashgate Research Companion to the Globalization of Health (2012) and co-editor of a four-volume collection of key sources in Global Health for the Sage Library of Health and Social Welfare (2011). Ted can be followed on Twitter @ProfGlobHealth.
Clare Bambra PhD is Professor of Public Health Geography and Director of the Centre for Health and Inequalities Research, Durham University (UK). Her research focuses on the health effects of labour markets, health and welfare systems, as well as the role of public policies to reduce health inequalities. She has published extensively in the field of health inequalities including a book on Work, Worklessness and the Political Economy of Health (Oxford University Press, 2011). She contributed to the Marmot Reviews of Health Inequalities in England (2010) and Europe (2013); the US National Research Council Report on US Health in International Perspective (2013); a UK Parliamentary Labour Party Inquiry into international health systems (2013), as well as the Public Health England commissioned report on the health equity in the North of England: Due North (2014). She is a member of the British Labour Party and can be followed on Twitter @ProfBambra.
