Delivering healthcare fit for a liberal democracy in the 21st Century.
This policy document was prepared for a Liberal Democrat Policy Working Group after wide consultation among healthcare professionals and health policy experts. It has wide support within the Liberal Democrat Party but has not been endorsed by the Party or the Party Leadership.
Problems the NHS is facing:
- Doctors and nurses are burdened with ever increasing bureaucracy
- Targets have led to box ticking rather than taking care of patients
- Services are less and less joined up from the patients’ point of view
- There is less and less money to spend
All these issues put pressure on staff to deliver according to contracts, targets and statistics.
As a result staff morale is plummeting and the quality of care is seriously under threat.
We propose to:
- return the focus to care of the patient
- give Local Health Boards the power to ensure care is integrated and co-ordinated
- give genuine choice to patients and their GPs
- make savings in bureaucracy amounting to 25% of projected NHS expenditure.
The National Health Service in the United Kingdom owes its existence to the vision courage and determination of three great politicians. David Lloyd George, prepared the ground with his 1911 National Insurance Act, and William Beveridge, who made the intellectual case for its creation. It was introduced in 1948 thanks to the determination and courage of the Minister of Health Aneurin Bevan. At a stroke, the United Kingdom provided health care for everyone, making it one of the first countries to do so. In contrast, some of its continental neighbours, which clung to their inherited social insurance systems, took much longer to achieve universal coverage, and the USA still fails to provide universal care.
The beauty of the system designed by Beveridge was its simplicity. Funded by taxation, there was no need to create separate, costly, and complex mechanisms to collect the money to pay for it. Access to all meant that there was no need to create an expensive, intrusive, and discriminatory system to check entitlement to care. Public sector provision reduced the scope for opportunistic behaviour by those who would seek to profit from illness, while encouraging a strong public sector ethos characterised by commitment and altruism. Indeed, although he could not have realised it, Beveridge’s thinking was far ahead of its time. It was only many years later that economics Nobel laureates would provide the theoretical and empirical basis for his ideas, such as Kenneth Arrow who, in 1963, showed why markets in health care fail and Oliver Williamson who showed the problems that arise in markets where the product cannot easily be specified and there is scope for opportunism (features that characterise much of health care).
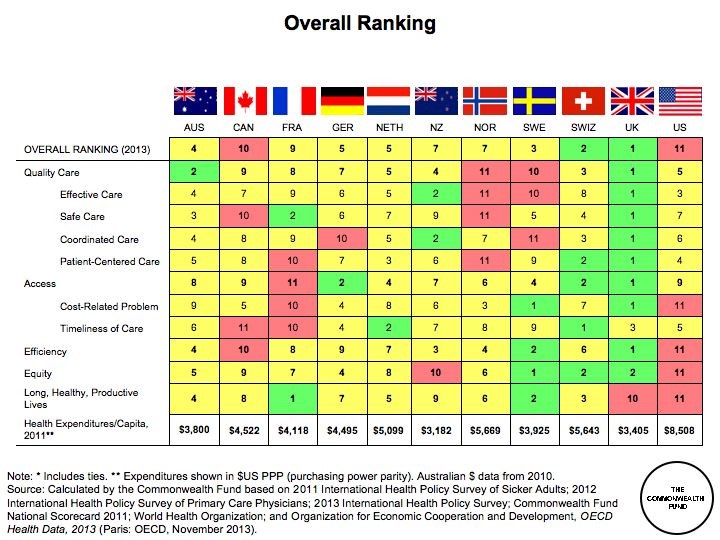
The result was a health system that was widely admired internationally and has been emulated by others. When Southern European countries, such as Spain, Italy and Portugal saw the need to reform their health systems in the 1980s they looked to the United Kingdom and other systems that employed a similar model[i]. Their decisions have been justified; the UK, along with these similar systems, consistently rank very highly in international comparisons such as those conducted by the New York based Commonwealth Fund,[ii] [iii] [iv] and the OECD.[v] [vi]
This does not mean that the NHS does not need to change. It does, as does every health system. The NHS faces demands caused by more expensive technology and drugs (the main driver of rising costs), ageing populations (who are not necessarily more expensive but who do have more complex problems), and changing expectations (although also often exaggerated). Nor has the NHS been perfect; it has been criticised for too much centralisation and some high profile lapses in quality of care. Yet those who call for constant change seem unaware that it has been changing. Indeed, it has been among the most successful health systems in responding to the growing challenges of chronic diseases, with outcomes in diabetes among the best in the world, and its response to the emergence of HIV/AIDS is widely admired. The UK was also in the forefront, internationally, in the move to day surgery. But there is always more to do.
And the NHS could have done better in some ways. It has had an historic problem with waiting lists, though these were largely eliminated between 2000 and 2010. In some cases services were less responsive to the expectations of patients than they should have been. Cancer outcomes, which depended on access to very expensive equipment and specialist expertise, lagged behind those in many other countries, as did some causes of death amenable to timely and effective care. Of course there were a number of reasons but perhaps the most important was that the NHS had been run on the cheap. Although the intrinsic efficiency of a tax-based, publicly delivered system meant that it was cheaper than more market-oriented systems, successive governments were unwilling to devote the resources it needed. Spending was consistently well below the European Union average as a share of GDP[vii] whilst retaining 100% public coverage. Indeed, once spending increased, in 1999, waiting lists fell, outcomes improved, and satisfaction among the public reached an all time high.
Despite having performance that was good by international comparisons the last thirty years has seen repeated reorganisations in the pursuit of greater efficiency. This might be acceptable had those reorganisations been based on evidence that they would make things better. But they weren’t. Running through them was a quest to encourage a plurality of providers using market competition, despite the mass of evidence of market failure in healthcare particularly in terms of reducing health equity and quality[viii] [ix]. Worse, many of the changes were introduced without an electoral mandate and without consultation of those who work in the system and have undermined the very public service ethos which has underpinned the NHS.
Paradoxically, these changes have made it more difficult for the NHS to adapt to the very pressures they were meant to address. We know that the existing pattern of hospital provision needs to change. Some hospital facilities are in the wrong place, and with increasing sub-specialisation and the importance of consultants of different specialties having close contact and support from other specialties some reconfiguration is essential. Quality healthcare increasingly needs to be delivered from larger units. The very nature of a competitive market promotes duplication and fragmentation. To have competition between providers there must be more than one provider. Opening the market to ‘any qualified provider’ is designed to increase the number of providers. As each provider is autonomous they will choose what services they offer. A provider cannot be forced to deliver a service that they are unwilling or incompetent to provide. Fragmentation is incompatible with either efficiency or high quality. The meaning of ‘local’ in terms of healthcare provision is changing. Yet it is now becoming impossible to bring this change about in a sensible way. Take the proposed downgrading of Lewisham Hospital, a decision that made no sense and was overturned in the courts, with the judgement suggesting that the Secretary of State failed to understand the legislation his predecessor had introduced. Or Poole and Bournemouth, where almost everyone agrees that two hospitals should merge, except for the competition authorities charged with creating a market where none should exist. Local services need to be under local control and aggregated to a level more appropriate to the provision of a full range of integrated services. Only by doing this can we deliver integrated care both to individuals and to local populations. (See proposal 1.)
Using targets and contracts in the pursuit of efficiency takes the focus off the needs of the patient. In effect the system may become more efficient at delivering something that is not fit for purpose: it is not what the patient wants or needs. This creates a great increase in activity, but it is non-productive activity; described by John Seddon as ‘failure demand’.[x]
Even worse, the huge transaction costs involved in creating an artificial market are sucking resources out of the NHS at a time of unprecedented pressure on government resources.
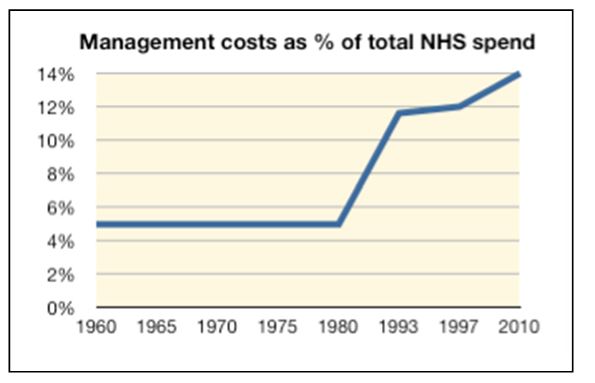
NHS administration costs prior to the introduction of the internal market were 5%.[xi] After 1981 and the introduction of the internal market administrative costs soared; in 1997 they stood at about 12% and by 2010 costs had risen to 14%.
Between 2000 and 2010, as the Labour government placed more and more contracts with external providers, the number of NHS managers increased twice as fast as the number of doctors[xii] and five times the number of nurses[xiii].
Both Conservative and Liberal Democrat Parties criticised the increase in NHS management costs under Labour and the current government claimed that the Lansley reforms would reduce management costs. Unfortunately that promise is most unlikely to be delivered[xiv]. Far from reducing the number of NHS organisations the number has increased not least because PCTs were replaced by CCGs which have a smaller geographical coverage. This will increase costs as economies of scale in commissioning could be lost.[xv] All the evidence suggests that increasing market competition and complexity will increase administration and management costs.[xvi] This increase in cost is accompanied by no increase in choice, quality or equity.
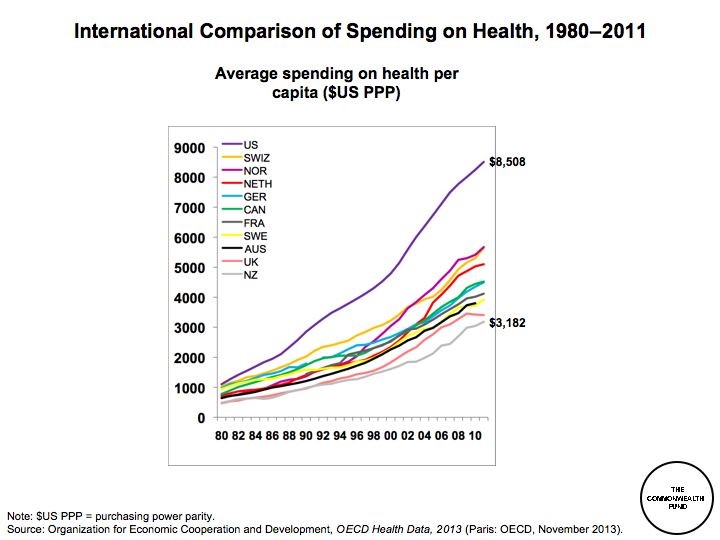
In the US In 1999, administrative spending consumed at least 31.0% of health spending[xviii] [xix]. Billing alone cost up to 13%. It is worth noting that the billing costs in healthcare providers are ten times the average of all businesses in the US.[xx] There is an inherent complexity to the business of delivering healthcare.Administrative costs in countries with a purchaser/provider split and a mix of state and private insurance tend to be higher still, purchaser costs alone typically amounting to around 20%[xvii] .
In March 2010 the Health Committee report on Commissioning concluded that ‘the purchaser/provider split may need to be abolished.’[xi] (See proposal 9.)
Governments have frequently claimed that the NHS did not need more money, but that it need to use what it had more efficiently. We understand that we cannot have something for nothing. The NHS must be properly resourced and seek maximum efficiency. OECD countries typically spend 8% of GDP on healthcare. The Conservative government between 1980 and 1989 presided over a decline in net UK spend on health from 5% to 4.5% of GDP at the same time as requiring frequent costly management changes and increased bureaucracy. The Labour governments between 1997 and 2010 increased spend on the NHS from 5.3% to 8.5%. The spend was concentrated on revenue and minor capital. By 2010 waiting lists were low and public satisfaction in the NHS was at an all-time high. Unfortunately the Blair/Brown partnership has saddled the NHS with crippling debts though numerous ill-conceived Private Finance Initiative (PFI) schemes.[xxi] [xxii] [xxiii] In the mistaken belief that debts incurred under PFI schemes would not appear as government debt, hospitals were forced to undertake building schemes financed by complex long-term contracts. At a time when the government could borrow at 6%, PFI schemes were committed to paying around 16% and also had to take on long-term service-contracts for services that may well be irrelevant well within the life of the contract. Hospitals need to be relieved of the crippling repayments required by PFI schemes. (See proposal 10.)
And it is not even clear that any of this will work in the way that it was sold to the public. The current system was meant to place GPs in the driving seat of the NHS. Yet, once a few of them had been persuaded to support this idea so as to get the Bill into law, they find themselves under sustained attack, portrayed in government briefings as the problem, not the solution. Inevitably, many are walking away, leaving the commissioning process to be swallowed up by the soon to be privatised Commissioning Support Units. These units bring additional cost burdens to the NHS and as private companies have no democratic accountability. (See proposal 13.)
It was also claimed that the reforms would increase patient choice, allowing them to decide where they would like to be referred for treatment. In reality, an increasing number of Commissioning Groups are not even giving them the choice to have treatment at all, refusing referrals for conditions such as hernia, varicose veins and hip or knee operations. The only choice patients have then is to pay for treatment or to go without. (See proposal 11.)
A further threat to the introduction of integrated care arises from the breakdown in professional co-operation that used to exist between and within specialties. International studies of similar reforms have shown a decrease in health care equity.8 (See also Francis report 29.)
Public Health is another area of concern. Despite claims to strengthen Public Health[xxiv] [xxv] the result has been fragmentation and confusion. Parts of Public Health are now with CCGs, parts with Local Authorities, parts with Public Health England (a new agency within the Department of Health). There are more senior public health professionals working in hospital trusts than in Local Authorities and CCGS combined[xxvi]. In addition the Secretary of State has new responsibilities for Public Health. There must be concerns about the ability of such a fragmented organisation to co-ordinate planning for whole populations or to the control of infections such as TB. The UK has almost the highest incidence of TB in Western Europe.[xxvii] (See proposal 7.)
It is a matter of great concern that the pursuit of market competition is militating against the delivery of good quality integrated care. At a time of ageing populations and multiple pathologies delivering integrated care is increasingly important and rightly recognised as being so. Market competition acts as a barrier to the rapid dissemination of good practice, impedes the free flow of information about patients from one provider to another and inhibits the co-operation of specialists across providers. Sir David Nicholson, chief executive of NHS England has said that the new competition rules are a barrier to delivering quality in the NHS[xxviii]. The Torbay model of integrated health and social care – which is held up as an example of best practice – has been referred to Monitor as potentially anti-competitive. Would-be private providers are able to invoke the law to obstruct good practice. The appalling lapses of care seen at Stafford were in large part due to the misguided pursuit of business models demanding a balance between income and expenditure. The Francis report draws attention to the way in which competition had eroded collegiality and trust[xxix].
The fragmented NHS driven by market competition is also a barrier to fairness and equity. There has always been a tendency for areas of high population density to benefit from a wider range and greater supply of services. There is evidence that increasing use of competition is increasing levels of inequality.8 25 Experience of other privatised services has also show an increased concentration of services in centres of high population at the expense of more rural parts of the country.
These concerns, to deliver a high quality, integrated, equitable and efficient healthcare service all drive our current proposals.
Proposals
Our proposals for the NHS are straightforward, evidence-based and simple. They build on the best features of the current NHS and embrace long-standing principles of equity, localism and choice.
- We will bring together all the NHS Trusts and Foundation Trusts in a locality under the management of a Local Health Board. This will create a single organisation that delivers integrated care covering hospital, community and mental health care.
- Health and Well-being Boards (H&WBB) have local representation but no power to deliver. Clinical commissioning Groups (CCG) bring clinical expertise but have no democratic accountability. We would establish Local Health Boards each covering a population of around 1,000,000. Initially these Local Health Boards would draw their membership from the current H&WBBs and CCGs. Over a period of five years Local Health Boards would move towards a more directly democratic composition.
- The assets of all NHS Trusts and Foundation Trusts would transfer to the Local Health Board for that area thereby allowing local services to be developed and delivered in the way most suitable to that locality.
- Local Health Boards would directly manage the contracts for local pharmacies, opticians, dentists and GPs[xxx]. In APMS[xxxi] practices, GPs and all staff would be directly managed by the Local Health Board.
- Local Health Boards would be grouped into regions and would be overseen by a Regional Health Authority who would distribute resources to each Local Health Board based on a capitation allowance for the whole population of that locality.
- Regional Health Authorities would in effect combine some of the functions of the current regional offices of NHS England and specialised commissioning hubs run by NHS England. Specialist Services that cannot be safely or appropriately delivered for a population of around 1,000,000 would be provided by the Regional Health Authority who would arrange for such services to be delivered from within one or more of the hospitals in that region. The number of Regional Health Authorities is yet to be agreed. NHS England has four regions, 10 specialised commissioning hubs and twenty-seven Areas. There are six BIS offices, and there used to be nine regions in the NHS.
- A supra-regional specialty committee would be set up nationally with members appointed from each of the Regional Health Authorities. This committee would agree arrangements for the provision of those services that are so rare that they can only be provided or planned for on a national basis.
- We shall consult more widely on the further integration of Public Health, but as a first step local Directors of Public Health would become members of the Local Health Board.
- We would abolish the market in healthcare within the NHS thereby removing the need for tendering, commissioning and contracting, monitoring contracts, invoicing and paying of bills. This is expected to save around 25% of expenditure.
- All PFI debts held by NHS Trusts would be pooled and held nationally in line with recent Treasury guidance[xxxii]. This would remove the distortion between different hospital trusts and make it easier to refinance, re-negotiate or pay off the debts.
- Patients would be given the choice, through their GP, of being referred to any consultant in the country. As no money changes hands there would be no need for complex contracting arrangements and whether or not the referral and treatment goes ahead would depend solely on the capacity of the receiving hospital to take on the work.
- These proposals would address the greatest single threat to the ability of the NHS to deliver a high quality and affordable service to all. But they do not address all the problems in our current complex and fragmented care services. There remain barriers and boundaries between health and social care and between hospital and community services. These barriers make for inefficiency in the service and frequently prevent the patient or client from receiving the care that they need. A major block to the integration of health and social care has been the fact that health care is provided free of charge, whereas social care is means tested. The implementation of the proposals of the Dilnot commission would largely address this issue. We would, therefore set up a commission to explore a system redesign to enable community care, social care and hospital care to be provided in a genuinely seamless way. Only then will the Local Health Boards truly earn the description of Local Health and Well-being Boards.
- By removing the burden of commissioning and contracting and by introducing direct management of hospital trust the workload of some NHS bodies would be radically reduced. Some bodies would in effect have no function. We shall discuss further before abolishing these quangos, but likely candidates would include: NHS England, and many of its substructures (it currently has its 4 sectors, 10 specialised commissioning hubs and 27 teams.) Monitor, the 17 Commissioning support units and the Trust Development Authority.
These proposals will empower patients and the healthcare professions. They will increase local involvement and give a sense of local ownership in the managing of the health services. They will enable the delivery of a fair and equitable service to all patients regardless of geography or medical specialty. They will facilitate a truly co-operative and integrated service as different specialists and hospitals will no longer be in competition with one another; patients can be treated by the specialist most able to help them and the sharing of knowledge and expertise can become routine. Finally, and importantly they will save money.
References
[i] Canada, Australia, New Zealand and Scandinavia.
[ii] Davis et al. Mirror mirror on the Wall: an international update on the comparative performance of American healthcare. Commonwealth Fund May 2007
[iii] Davis et al. Mirror mirror on the wall: How the performance of the US healthcare system compares internationally. Commonwealth Fund June 2010
[iv] Davis et al. Mirror mirror on the wall: How the Performance of the U.S. Health Care System Compares Internationally. Commonwealth Fund June 2014
[v] OECD. UK ranked number 1 in Unmet care need due to costs in eleven OECD countries, by income group, 2010 Health at a Glance 2011: OECD Indicators- http://dx.doi.org/10.1787/888932525666
[vi] OECD. UK ranked number 1 in Out-of-pocket medical costs 2010, Health at a Glance 2011: OECD Indicators http://dx.doi.org/10.1787/888932525761
[vii] OECD. Health expenditure as a share of GDP, 1960-2009
[viii] Bambra, Garthwaite, and Hunter, All Things Being Equal: Does It Matter for Equity How You Organize and Pay for Health Care? A Review of the International Evidence Int. J. Health Serv. 44(3):457-477, 2014
[ix] Footman, Garthwaite, Bambra, and McKee Quality Check: Does It Matter for Quality How You Organize and Pay for Health Care? A Review of the International Evidence Int. J. Health Serv. 44(3):479-505, 2014
[x] Seddon J, Systems thinking in the Public Sector: Triarchy Press. passim.
[xi] House of Commons Health Committee HC 268-I Published on 30 March 2010
[xii] http://www.telegraph.co.uk/health/healthnews/7213118/NHS-managers-numbers-rise-at-twice-rate-of-doctors-report-finds.html
[xiii] http://www.theguardian.com/society/2010/mar/25/nhs-management-numbers-frontline-staff
[xiv] http://www.ft.com/cms/s/0/23e48198-e845-11e0-9fc7-00144feab49a.html#axzz2g88lFHBA
[xv] http://www.gponline.com/News/article/1190046/Watchdog-reveals-11bn-cost-NHS-reforms/
[xvi] Woolhandler S, Himmelstein D, Competition in a publicly funded healthcare system BMJ 2007;335:1126
[xvii] http://www.who.int/health_financing/documents/dp_e_10_08-admin_cost_hi.pdf
[xviii] Himmelstein D U, Woolhandler S, & Wolfe, S. M. Administrative waste in the US health care system in 2003: International Journal of Health Services, 34(1), 79-86.
[xix] Woolhandler et al Costs of Health Care Administration in the United States and Canada: N Engl J Med 2003;349:768-75.
[xx] http://www.ncbi.nlm.nih.gov/books/NBK53942/
[xxi] Gaffney D, Pollock AM, Price D, Shaoul J, PFI in the NHS – is there an economic case? BMJ 1999;319:116
[xxii] Gaffney D, Pollock AM, Price D, Shaoul J, NHS capital expenditure and the private finance initiative—expansion or contraction? 1999;319:48
[xxiii] Smith R, PFI, perfidious financial idiocy, BMJ 1999;319:2
[xxiv] Healthy Lives, Healthy People: our strategy for public health in England DoH Nov 2010
[xxv] Davies S, Marsland A Public Health System Reform: DoH 20 June 2011
[xxvi] Faculty of Public Health. Personal communication.
[xxvii] WHO ‘Global tuberculosis report 2012’
[xxviii] Iacobucci G, Competition is holding back quality improvements, says NHS boss BMJ 2013;347:f5862
[xxix] http://www.midstaffspublicinquiry.com/report
[xxx] The majority of GPs are employed under General Medical Services contracts (GMS) and are independent contractors within the NHS. This would not change. GMS GPs employ their own staff.
[xxxi] Alternative Provider Medical Services
[xxxii] HM Treasury: A new approach to public private partnerships Dec. 2012