Within the Osier paradigm, doctors have generally accepted accountability in two directions; to their professional colleagues collectively, and to their patients individually. In each case, accountability has been at two levels: a formal level of official complaint, disciplinary action or litigation; and an informal level of custom and expectations.
Because in Osier’s time doctors had so little influence on the outcome of illness, accountability for outcome was not possible. Even the traditional Hippocratic rule ‘primum non nocere’ (above all, don’t harm) was not enforceable; desperate fear condoned desperate remedies; so doctors were encouraged to add substantial risks from treatment to the uncertain but often serious risks of illness. The dangers of surgery were obvious, but less well remembered are the often highly toxic medicines in everyday use well into the 1940s. Strychnine, lead, arsenic and mercury were common ingredients of pills, medicines and ointments used for a wide variety of conditions for which no treatment of experimentally proven effect was available. Doses were supposed to be safe, but chronic lead and arsenic poisoning were common in sufferers of multiple sclerosis, motor neurone disease, migraine, trigeminal neuralgia, hysteria and other chronic disorders for which they were often prescribed. When I was a medical student in 1950 ‘pink disease’, an often fatal disorder of infants, was proved (after prolonged and acrimonious controversy in the medical journals) to be chronic mercury poisoning from teething powders, prescribed by doctors or bought over the counter from chemists.
When the Osier paradigm was developed, transactions between doctors and patients were largely illusory. Then as now, they were seldom consciously deceptive. The chief therapeutic agent, and the chief product of a medical consultation, was hope, and doctors and patients collaborated more or less equally in producing and sustaining it. There was a tacit social agreement that the alleged centre of the medical process (attempts to alter the course of illness) could not be subjected to serious direct criticism, because then there would soon be no profession left to criticize. Credulity was an important part of the medical process, valued by patients as much as by doctors, and this was the principal justification for the very tight definition of medical privilege and exclusion of competing skills. Instead, criticism was focused on the medical process rather than its outcome. The most dependable defence was strict adherence to conventional process, not only clinical process but also the ways in which doctors dressed, spoke and behaved. Outrageous social behaviour and barefaced fraud were the main targets; not what doctors did, but how they did it.
This refusal to look objectively at the clinical centre of medical failure and success, at the overall gains or losses in long-term health and happiness, is still with us. Despite massive evidence that effective medical knowledge is very incompletely applied, this hardly figures in the personal accountability of doctors for their daily work. Instead, we maintain systems for chasing exceptional offenders accused of exceptional crimes, while leaving the effectiveness of our daily work unmeasured and largely unknown.
Accountability to Professional Bodies and Administration
Professional accountability in Britain is to the General Medical Council (GMC), representing a mixture of lay and professional establishment opinion, with its own disciplinary powers to suspend or expel doctors from their profession, outside the ordinary legal system. Similar European bodies, like the Ordre des Medecins in France and Belgium, combine these powers with representation of the real or imagined interests of doctors in negotiation with the State, reinforcing the power of established doctors to restrict social innovation within the profession. In Britain this negotiating function has always been carried out by the BMA, distantly flanked by the minuscule MPU, without disciplinary powers or compulsory membership.
In 1983, 920 doctors out of about 60,000 in all forms of practice were reported to the GMC for suspected misconduct. Only 40 of these were ultimately referred to the Professional Conduct Committee. The most that can be said for the GMC is that it sets an outer limit to professional negligence or incompetence, but this is so remote from everyday success or failure that it is of little interest to doctors concerned (as the vast majority are) with the effectiveness of ordinary care.
Formal complaints by patients about doctors either in hospitals or general practice are infrequent. The Royal Commission on the NHS ( para. 11.12. Cmnd 7615, London: HMSO, 1979.) recorded that of about 200 million patient contacts with GPs in 1978, only 1,465 led to formal complaints to Family Practitioner Committees. Complaints about doctors in hospitals were more frequent, but of six million in-patient treatments and nine million new outpatients in that year, less than 1% led to written complaints. In 1983 there were about 19,600 written complaints about hospital care, about one in 2,000 episodes of treatment. (Capstick, B., Patient complaints and litigation, Birmingham: National Association of Health Authorities in England & Wales, 1985.) Less than half of these were complaints about clinical management.
The NHS remains a popular service, and those who work in it are still generally well thought of. However, in a retrospective analysis of 500 consecutive deaths in my own practice from 1964 to 1985, I was able to identify avoidable factors in 45%, of which 59% seemed mainly attributable to the acts and omissions of patients, 20% to misjudgements by myself and my GP colleagues, and 4% to misjudgements and errors by hospital doctors, though it was difficult to get as much information about the last category as I had about myself and my colleagues. (Hart, J.T., Humphreys, C., ‘Be your own coroner: an audit of 500 consecutive deaths in a general practice’, British Medical Journal 1987; 294:871-4.) I have no reason to believe these figures are unusual, so evidently few events deserving (hopefully constructive) criticism lead to any formal complaint. I do not, of course, suggest that they should, but a mature science should be founded on self-criticism and mutual criticism, in which doubt rather than faith is the accepted norm, not in order to pillory malpractice, but to advance the practice of scientific medicine. Our existing machinery of criticism is almost entirely irrelevant to this aim, and lags far behind the real moral position already attained by most doctors.
In hospitals, where doctors are salaried and their work is at least nominally co-ordinated within teams and between specialties, NHS administration has in practice little to do with maintaining standards of medical care, except in this negative and exceptional sense of fielding complaints. Even then, accountability of consultants is unconvincing. In an editorial in the British Medical Journal, (Drife, J.O., ‘Consultant accountability’, British Medical Journal 1987; 294:789-80.) a teaching hospital consultant has described and explained the problem:
In hospitals administrative staff are accountable to general managers and nurses to the District Nursing Officer, but the accountability of doctors is not clear. Hospital doctors in training are answerable to their superiors, but after being appointed consultant. . . a doctor has a secure job and does not appear to be accountable for the quantity or the quality of his work.
There are several reasons for this. One is historical: years ago consultants gave their services free to charitable institutions, which could hardly complain when the consultant was not in constant attendance. The influence of this tradition persists, and some consultants still think that their main clinical job is simply to be available for consultation to junior staff. Another reason is that consultants—unlike senior nurses—have a mixture of clinical and administrative responsibilities, which are closely interlinked. It is difficult for an employer to make a consultant accountable for administration while deferring to him on clinical matters, and the question of clinical accountability is a sensitive one.
Even more in general practice than in hospitals, most complaints concern style rather than clinical management, probably because in this area patients have more confidence in their own judgements. Klein (Klein, R., Complaints against doctors, London: Charles Knight, 1973.) reviewed complaints to Family Practitioner Committees (FPCs) in 1973. Nearly 35% were about GPs’ or their receptionists’ manners and remarks, 22% were about delays in visiting or problems about appointments and only 11% were about diagnosis or treatment. He noted that whereas doctors seemed mainly to fear and organize to defend themselves against accusations of clinical incompetence, patients actually complained mainly about how GPs, hospital doctors and their office and nursing staffs treated them as people, though they may rightly have believed that rudeness and secrecy may have serious clinical consequences.
Litigation
Litigation by patients and their relatives for medical malpractice, though rising, remains uncommon in the NHS. An estimate for 1983 was that only about 5% of formal complaints resulted in writs for damages, of which 30-40% were successful. (Capstick, B., Patient complaints and litigation, Birmingham: National Association of Health Authorities in England & Wales, 1985.) This is in striking contrast with the USA, where in 1986 18.3 claims were made for every 100 insured physicians, and sums awarded in compensation were vastly greater than in Britain. The reasons for these differences are complex. In a careful analysis, Quam, Dingwall and Fenn (Quam, L., Dingwall, R., Fenn, P., ‘Medical malpractice in perspective. I. The American experience. II. The implications for Britain’, British Medical Journal 1987; 294:1529-32, 1597-1600.) pointed out that:
In principle the National Health Service seems likely to reduce claims in at least four ways: there is no direct cost to the patient for extra medical care to remedy an injury; access to care is guaranteed throughout life; there is no direct financial relation between doctors and patients; and the system of referral restrains specialists while encouraging loyalty between patients and their general practitioners.
However, they go on to warn that all these supportive features could be lost.
. . . unless the level of National Health Service resources is seen to be adequate to ensure reasonable access and treatment, so that there is no need to litigate for funds to purchase care…
and that:
The present constraints on National Health Service funding may by their pressure on medical personnel, also precipitate an increase in the number of incidents capable of leading to claims. . . Fatigue is not a legal defence against an allegation of negligence. Similarly, if junior doctors take on work beyond their level of skill and experience they cannot rely on this as a defence. There is only one legal standard of care: if a doctor is not sufficiently experienced to perform a particular procedure he or she should not undertake the work. Obviously, it is difficult to insist on this when faced with pressing clinical needs, but then the risk of litigation must be evaluated as a cost of a system which requires young doctors to work long hours with limited senior cover.
Whether lawyers accept it or not there are different clinical standards in general practice (particularly industrial working-class practice) on the one hand, and in hospitals on the other, and many GPs as well as young doctors in hospitals work long hours isolated from peer criticism. All evidence suggests that the relative immunity from formal complaint and litigation of British doctors, and particularly of British GPs, has depended on the gratitude and loyalty of the public and its low expectations in a free but always overworked and underfunded State service. Recent evidence from the Social and Community Planning Research (SCRP) surveys (Jowell, R., Airey, C., British social attitudes: the 1987 report, Aldershot: Gower Publishing, 1987.) on public satisfaction with the NHS, shown in Table 7.1, gives no ground for complacency.
Table 7.1 Public satisfaction with the NHS
| Survey year: | 1983 | 1984 | 1986 |
| Very satisfied |
11% |
11% |
6% |
| Quite satisfied |
44% |
40% |
34% |
| Neither satisfied nor dissatisfied |
20% |
19% |
19% |
| Quite dissatisfied |
18% |
19% |
23% |
| Very dissatisfied |
7% |
11% |
16% |
In the same study, dissatisfaction (quite or very dissatisfied) in 1983 (Jowell, R., Airey, C., British social attitudes: the 1984 report, Aldershot: Gower Publishing, 1984.) rose from 21% of those with annual incomes under £5,000 to 34% of those with incomes over £10,000; 13% of all respondents were dissatisfied with the GP service, compared with 7% for hospital in-patient services and 21% for hospital out-patient services. Patients, particularly younger and richer patients, are becoming more critical, and possibly more litigious.
Accountability to Colleagues
More perhaps than anything else, medical students learn to respect clinical competence, a term frequently used by doctors but difficult to define. In the sense in which it is usually understood, it need not include several features essential to effective medical care. We all understand what is meant by describing a doctor as clinically competent, but so rude and unsympathetic to patients that this competence cannot be effectively expressed. Competence always includes knowledge of the biological aspects of disease, and the technical means of dealing with it, but understanding of people, even as necessary vehicles for disease, is a desirable but not essential extra.
Clinical competence is the currency in which all kinds of intraprofessional negotiations and conflicts are conducted. A woman doctor in the USA quoted by Good (Good, M. J.D., ‘Discourses on physician competence’. In, Hahn, R.A., Gaines, A.D. (eds.), Physicians of Western medicine, 247-67. Boston, Mass.: D. Reidel Publishing, 1985.) expresses this idea of currency very perceptively:
I think for a long time I tried to increase my competence, or my vision of myself as competent, or other people’s visions of me as competent, at the expense of other physicians’ competence. I think that’s what a lot of doctors do. It’s like there is only so much competence in this world. If I have more, they have less; if they have more, I have less.
Clinical competence, in other words, is like other kinds of wealth and power. There must be winners and losers; we all love winners, nobody likes losers. Forget about our profession as a band of brothers and sisters in service to mankind, it’s just another part of the universal war of every man against every man. Incompetent doctors are, like incompetent patients, simply rubbished.
In this view medicine is predatory, and the most successful doctors can be judged only by others who have shed blood in the same way. In 1984 Dr David Kinzer (Kinzer, D.M., ‘Physicians as fighter pilots’, New England Journal of Medicine 1984; 311:206.) reiterated an opinion he first published in 1959, that the needs of physicians are best understood as resembling fighter pilots in the Second World War:
Relating to my combat experience flying dive bombers and fighter planes, the success or failure of our performance was measured in one-to-one situations. No dive-bombing run on an enemy ship or dogfight with an enemy plane was like any other. It was always a very lonely experience. The carrier we took off from and, we hoped, would land back upon was always, during these moments, a remote and almost irrelevant entity. . . An explicit reality here is that the missions of the pilot and the carrier were not the same, nor are the missions of the hospital and the clinicians on its medical staff. This distinction is important. The carrier (or the hospital) is an organization whose only reason for being is to provide a support system for the missions of its pilots (or physicians). Whether the mission is a dogfight or a critical trauma case, it is still the prime responsibility of the pilot or the attending physician. The organization, with its technical hardware, supply system, and support personnel, has only a backup role.
This view is typical of the way in which junior hospital doctors see themselves and their work. Mizrahi and colleagues (Mizrahi, T., ‘Managing medical mistakes: ideology, insularity and accountability among internists-in-training’, Social Science & Medicine 1984; 19:135-46.) studied 207 US hospital internists in residency training over a period of three years, using questionnaires and in-depth interviews to study their attitudes to accountability. Here are some typical statements, which could equally be heard from equivalent British resident staff:
As time goes on you don’t criticise as much because you know that you may have made the same mistake in the past. On the other hand you realise that you’re not going to change people if you criticise them. All you’re going to do is make them angry at you.
I remember my first patient who died that I felt in some way responsible. . . If I had done something differently maybe it would have made a difference. As a third year medical student, the patient had a bloody stool and my intern told me he was a ‘crock’ and not to be concerned.
Practically the first week I was on as a third year medical student, the chief resident told me a particular patient was a ‘SHPOS’ [Sub-Human Piece Of Shit]. I was there alone that night when he decided to crump [die]-. . . If I hadn’t been told he was SHPOS I might have gotten on the situation sooner.
I can’t say I have a whole lot of allegiance to anyone. I’m pretty much a loner. I feel accountable to myself and I feel accountable to try to do the best I can for the people I’m taking care of.
I’m accountable to me. Because it’s my job and I have chosen to do this to the best of my ability.
Mizrahi found that these completely doctor-centred views of accountability failed to convince even the doctors themselves:
Notwithstanding this shared elaborate repertoire of denial, discounting and distancing, it was found that profound doubts and even guilt remained for many housestaff. . For many the case was never closed, even as they terminated formal training… The house-staff ultimately sees itself as the sole arbiter of mistakes and their adjudication. Housestaffers come to feel that nobody can judge them or their decisions, least of all their patients. . . They have developed a strong ideology justifying their jealously guarded autonomy. In the graduate medical socialisation process, they have learned to believe that because they perceive themselves as their own worst judges, they should be their only judges. Because of the insularity and isolation of the housestaff subculture in a position of high prestige, with the power to make life and death decisions, they see themselves as singularly responsible for their actions and disparage any attempt by others to insert themselves into the process of accountability.
Kinzer and Mizrahi’s junior hospital doctors are talking about the USA, but what they say is easily recognized by doctors everywhere; the Osier paradigm of socially isolated, gentlemanly privilege is international. From their first day in medical school, doctors learn to see themselves as hunters, who know diseases as beasts in the jungle, and can shoot from the hip, hopefully hitting the disease more often than the patient, but accepting that hunting accidents are in the nature of the game and are bound to happen. It may be dangerous for patients, but it’s also dangerous for doctors. In a study of 170 junior house officers in British Hospitals, Jenny Firth-Cozens (Firth-Cozens, J., ‘Emotional distress in junior house officers’, British Medical Journal 1987; 29:533-6.) found that 50% reported emotional disturbance arising from stress, mostly overwork and loss of sleep. 28% showed evidence of depression on psychiatric criteria, 19% drank alcohol heavily and 6% had suicidal thoughts. The study was prompted by two deaths from suicide in junior house officers.
Apart from crisis situations, the fantasy of doctors living dangerously as hunters, rescuing helpless and ignorant patients from attack by predatory diseases which doctors alone can recognize and understand, is an absurdity; but it is ideally designed for a service which abandons caring to concentrate on salvage.
The Patient’s Role in Diagnosis
Conan Doyle, a good middling doctor unable to make a living in Osier’s time, modelled Sherlock Holmes on an impressive teacher at his own medical school. Holmes was a stunning solo performer, creating a convincing diagnosis from whisps of this and crumbs of that, evidence available to the slower minds of his witnesses and to Dr Watson, but transformed by the great detective into creations entirely his own.
How Conan Doyle’s ideal managed to stage his apparently convincing performances only medical students familiar with the theatre of teaching consultancy can know. For most performers, some prior investigation and several rehearsals are necessary, with a spotlight blinding the captive audience to the equally essential contributions of the patient, nurses and junior medical staff. The solo consultant who can produce a dazzling diagnosis while making everyone else look a fool is as much a fictional character as Sherlock Holmes himself.
Consultation of a patient with a doctor for a newly presented complaint usually consists firstly of a diagnostic process (‘What’s wrong with this patient?’), then of a plan for treatment (‘What can be done to put it right?’). Objective studies of both these parts of a consultation show that patients as well as doctors must make active contributions of their own, if diagnosis is to be relevant to the patient’s problems and treatment is to be effective.
The diagnostic process usually has three stages: a history (what the patient says, mainly in response to a more or less systematic interrogation); physical examination; and laboratory, x-ray or other technical investigations. A group in Oxford (Hampton, J.R., Harrison, M.J.G., Mitchell, J.R.A., Prichard, J.S., Seymour, C., ‘Relative contributions of history-taking, physical examination and laboratory investigation to diagnosis and management of medical outpatients’, British Medical Journal 1975;irA86-9.) studied the relative importance of each of these to diagnosis by getting consultants to make a provisional diagnosis successively at each stage (after the history, after examination and finally after routine technical tests), and then comparing the proportion who reached the final diagnosis (made retrospectively at follow-up three months later) at each point. In 80 newly-referred medical outpatients, the final diagnosis was reached after reading the GP’s letter and taking the history in 66 (82%); physical examination added 6 (7%) and technical investigations added 7 (9%). Listening to the patient is not only more productive than these other more technical and perhaps more impressive processes, but is also essential to guide them in an intelligent direction; experienced doctors already have one or more hypotheses before they examine their patients to confirm or refute them, and their choice of technical tests similarly depends on hypotheses generated chiefly by the history.
‘Listen to the patient,’ said the great French 19th Century neurologist Jean-Martin Charcot, ‘he is telling you the diagnosis.’ Of course, patients cannot usually give a relevant history unaided, but the huge importance of their active, intelligent contribution only becomes obvious when because of cultural or language barriers, no history is available. Diagnosis and subsequent medical management then become veterinary rather than human, crude mechanistic interventions of value only in crises, when the patient’s role always tends to become passive.
It is doubtful whether Charcot fully understood the truth of his own aphorism. He is said to have refused ever to examine patients in a public teaching hospital unless they were stripped naked; only then, with a patient dumb with fear and shame before a hundred or more students, would he condescend to proceed with his examination. The social assumptions of Osier’s time made this conduct normal; sick people having free treatment in teaching hospitals were expected to speak only when spoken to, answering ‘yes’ or ‘no’ to cross-examination by the doctor, venturing no opinions of their own. Even when I was a clinical student in 1948-52 little of this had changed. Patients today are probably less willing to submit to such arrogance, but the problem is still recognizably there. Useful diagnosis is not just professional recognition of a biological process incomprehensible to the laity, but a useful analysis of interdependent problems which always (not sometimes) have multiple biological, psychological and social causes, all of which must be understood if we are to find effective solutions. To the extent that patients are discouraged from sharing in the definition of their medical problems, diagnoses will be made which are irrelevant to real lives, however biologically true they may appear to be.
A Clinical Example
As the antithesis of swashbuckling episodic battles with acute or end-stage disease, let me give an example of the sort of case where years, even decades of work are required, with less dramatic but probably more important results.
I have been responsible for primary medical care for Hopkin Morgan (the name is, of course, fictitious) since 1961, when I was 34 and he was 36. He’s a big man, a big soccer player in his youth, and a big coal miner who rarely missed a shift until a runaway tram gave him a compound fracture in one leg in 1964, and killed the man working beside him. A routine medical examination in 1960 had shown a blood pressure of 194/126 mmHg, but when this was repeated a couple of weeks later it had fallen to 168/94, still well into the top 1% of the distribution of blood pressure for a man of that age, but not high enough to justify treatment with the antihypertensive drugs available at that time. His blood pressure was not checked again until 1966, when two readings reached 200/120 and 170/120. He has at least nominally been on treatment with antihypertensive drugs ever since, and Fig. 7.1 shows in very simplified form what has happened since then to his weight and blood pressure, in relation to some other events.
Until his compound fracture he had no apparent medical problems. As there is no record of his blood pressure before 1960, there is no way of knowing how long it had been raised, but it was first recognized as a medical problem in 1966, though it was not causing symptoms. Evaluating his other risks for coronary heart disease, I found a blood cholesterol of 8.2 mmol/1 (318 mg/dl), a figure almost as exceptionally high as his blood pressure. The only good news was that he was a lifelong non-smoker. I also found persistent protein in his urine, suggesting some sort of kidney damage which might be causing his high blood pressure, so I referred him for investigation at a teaching hospital in 1967.
There he was found to have kidney damage from a raised level of blood uric acid, which can also cause kidney stones and gout (painful uric acid crystals in a joint, usually the big toe), though he did not yet have either of these. His kidney damage was severe enough to cause raised levels of metabolites excreted through the kidney, with blood urea concentrations averaging 52 mmol/1 (313 mg/dl). He was very overweight: six feet tall and weighing 103.4 kg. Like most miners, he was also a heavy beer drinker, getting through about 5 gallons a week according to his own probably modest estimate. Finally they confirmed an even higher blood cholesterol level of 9.5 mmol/1 (373 mg/dl).
In 1967 he therefore had the following inter-related medical and medicosocial problems, shown as reversible and for the most part measurable risk factors, together with their likely outcomes:
CURRENT PROBLEMS : PREDICTABLE OUTCOMES
Persistent disability from major compound fracture: Employment problems and loss of earnings
Very high blood pressure 200/120 mmHg: Early coronary heart disease, heart failure, and/or stroke
Very high blood cholesterol 9.5 mmol
High blood uric acid : Kidney stones and kidney damage potentially leading to kidney failure, joint damage from gout
High alcohol intake: Social damage at home and at work, obesity, further rise in blood pressure, further rise in blood uric acid
Obesity: Greater pain from old fracture, further rise in blood pressure, more joint damage, possibly diabetes
It is interesting to note how many of these outcomes were also potential causes, suggesting that early efforts put into control (Anticipatory Care) might yield disproportionately high dividends. His medical needs, his and my joint medical tasks, were optimal control of these risks to minimize or avoid these outcomes. He has now reached 62 years of age without angina, a heart attack, heart failure or stroke, and he has never had any important psychosocial problems from his heavy drinking. He has always had a strong, friendly personality, and his level of drinking, though a serious health hazard, is a cultural norm in a coal-mining community. His liver function, initially impaired (gamma glutamyl) transferase 250 units, about 200 units above the conventional upper limit) is now virtually normal (59 units). He did get repeated attacks of urate kidney stones in 1969 and 1970, but none since then, and his kidney function has been well preserved (blood urea in 1986 was 11.4 mmol/1).
On the other hand, his employment and other social problems were serious. After about a year off from his injury, no light work was available and he had to do heavy manual work in the coal washery which gave him a lot of severe pain. In 1970 his wife began to be seriously handicapped by chronic obstructive airways disease and emphysema, with three short admissions to hospital over the next five years. Eventually she became dependent on portable oxygen, and Hopkin gave up his work to look after her at home. She died in 1975. As you can see from Fig. 7.1, weight control was poor and in 1980 he developed diabetes, bringing a new set of risks of coronary heart damage, stroke, kidney damage, and eye damage. His diabetes has been well controlled on diet only, with glycosylated haemoglobin consistently below 9%.
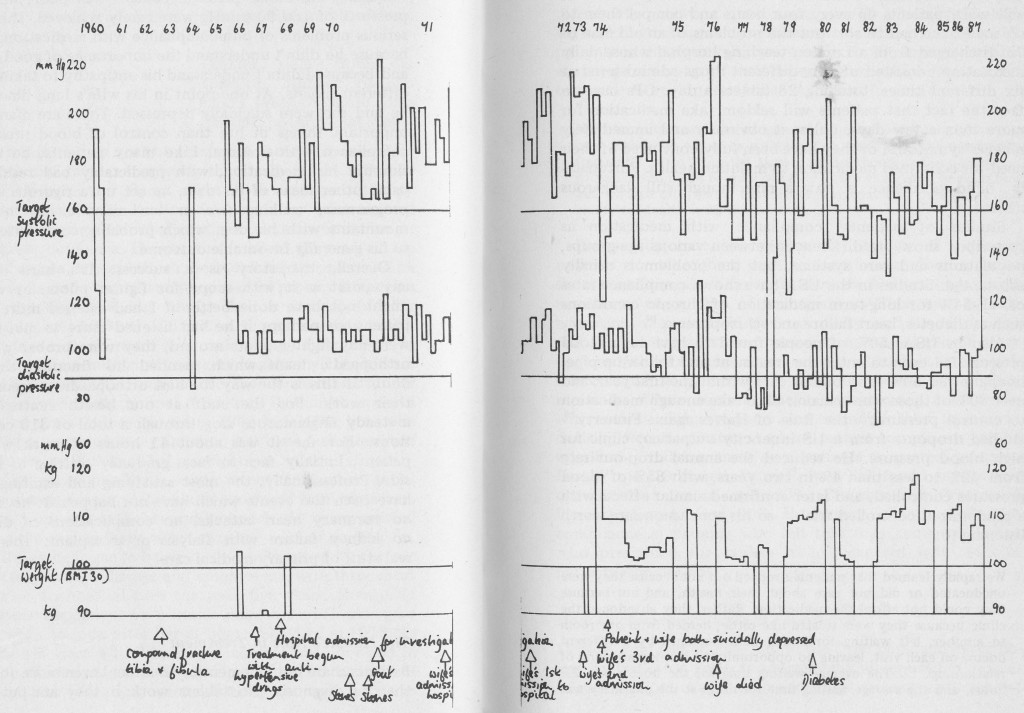
Quality of blood pressure control was poor; his target pressures of 160/90 mmHg were rarely achieved. There were serious problems of non-compliance with medication, at first because he didn’t understand the importance of good control and because I didn’t understand his antipathy to taking many different tablets. At one point in his wife’s long illness both he and she were suicidally depressed. There are many more important things in life than control of blood pressure or compliance with doctors. Like many patients, he tried to simplify his medication, with predictably bad results; but using other ideas of his own, he set up a rigorous exercise programme, walking five or ten miles a day over the mountains with his dog, which probably contributed a lot to his generally favourable outcome.
Overall, the story is a success. It’s hard to find any point in it with scope for fighter pilots, or where I might not have done better if I had listened more to the patient, or perhaps if he had listened more to me. If there were any fighter pilots around, they were probably on the orthopaedic team which mended his fracture, though I doubt if this is the way the best orthopaedic surgeons view their work. For the staff at our health centre it was a steady unglamorous slog through a total of 310 consultations. For me it was about 41 hours of work with the patient, initially face to face, gradually shifting to side by side. Professionally, the most satisfying and exciting things have been the events which have not happened: no strokes, no coronary heart attacks, no complications of diabetes, no kidney failure with dialysis or transplant. This is the real stuff of primary medical care.
The Patient’s Role in Treatment
Patients share in implementing treatment even more obviously than in diagnosis. No tablets work if they are put in the toilet instead of the patient. Hospital doctors dealing mainly with in-patients sometimes seem to imagine that whatever they prescribe will be taken, because a hierarchy of nurses will wake patients up every four hours and compel them to do so. I once had to sort out the problems of an old man of 75 discharged from a London teaching hospital whose daily medication consisted of nine different drugs administered at six different times, totalling 28 tablets a day. GPs have to face the fact that patients will seldom take medication for more than a few days, unless it obviously and immediately relieves symptoms, or they have been fully convinced of their need for continued medication to maintain health. Fortunately, blind obedience is now a rare though still dangerous disease.
Studies of patients’ compliance with medication as prescribed show big differences between various age-groups, populations and care systems, but the problem is usually substantial. Studies in the USA have shown compliance rates of 41-54% for long-term medication of chronic conditions such as diabetes, heart failure and schizophrenia. (‘Keep on taking the tablets: a review of the problem of patient non-compliance’, OHE Briefing no. 21, London: Office of Health Economics, 1983.)
Also in USA, 50% of people found to have high blood pressure fail even to enter the treatment and follow-up pipeline, another 50% drop out of care within the first year, and over 30% of those who remain fail to take enough medication to control pressure; (Sackett, D.L., Snow, J.S., ‘The magnitude of compliance and non-compliance’. In, Compliance in health care, ed. Haynes, R.B., Taylor, D.W., Sackett, D.L., p. 11. Johns Hopkins University Press, Baltimore, 1979.) the Rule of Halves again. Finnerty (Finnerty, F.A. Jr., Mattie E.G., Finnerty, F.A., ‘Hypertension in the inner city. I. Analysis of drop-outs’, Circulation 1973; 47:73.) studied dropouts from a US inner-city outpatient clinic for high blood pressure. He reduced the annual drop-out rate from 42% to less than 4% in two years, with 85% of blood pressures controlled, and later confirmed similar effects with a randomized controlled trial, (Finnerty, F.A. Jr., Shaw, L.W., Himmelsbach, C.K., ‘Hypertension in the inner city: II. Detection and follow-up’, Circulation 1973; 47:76-8.) so his conclusions are worth listening to:
We rapidly learned that patients dropped out not because they were uneducated or did not care about their health, and not because they could not afford the medication. Rather, they abandoned the clinic because they were treated like cattle, herded from one room to another, left waiting for hours, then examined by a different doctor on each visit, leaving no opportunity to develop any kind of relationship. . . The average waiting time for the doctor was 2.5 hours, and the average waiting time for drugs at the pharmacy was another 1.8 hours. . . In contrast. . . the average time actually spent with the physician was only 7.5 minutes.
Finnerty’s solution was to reorganize the clinic by developing an effective appointments system (average time spent by patients in the clinic fell from 4 hours to 20 minutes), and by ensuring continuity of staff-patient relationships. This turned out to be more important than staff qualification:
Most important was the assignment of every patient to his or her own paramedic whom he would see on every visit. The paramedics frequently came from the same neighbourhood as the patient.. . chosen not so much because of [their] prior experience or education but because of [their] friendly and sympathetic personality and ability to identify with the patients.
Perfunctory care has perfunctory results. If we want patients to take their treatment seriously, doctors must show that they take it seriously too, which means negotiating agreement on a plan of management. This must include education of patients in the reasons for, and the advantages and disadvantages of treatments recommended and of other options if there are any, and education of doctors on the real-life constraints within which patients have to apply their remedies. Where doctors develop a continuing relationship with patients, listen to them, and encourage them to share in devising realistic treatment plans, patient compliance can be excellent. Studying their own patients in general practice, Porter (Porter, A.M.W., ‘Drug defaulting in general practice’, Journal of the Royal College of General Practitioners 1969; 17:170.) in 1969 and Drury (Drury, V.W.M., Wade, O.L., Woolf, E., ‘Following advice in general practice’, Journal of the Royal College of General Practitioners 1976; 26:712-8.) in 1976 found medication compliance rates of over 80%. Ettlinger and Freeman (Ettlinger, P.R.A., Freeman, G.K., ‘General practice compliance study: is it worth being a personal doctor?’, British Medical Journal 1981; 282:1192-4.) likewise found over 80% compliance overall, and 91% compliance in patients who felt that they knew the doctor who prescribed the tablets well, compared with 44% in patients who did not.
How Doctors see Patients as a Resource
Doctors who still operate within the Osier paradigm nevertheless concede that patients are generally under-used as sources of information, that someone (perhaps some sort of attached social worker) should find out more about their social circumstances so as to avoid the more nonsensical consequences of treating diseases rather than people, and that the necessary education of patients in the nature of their treatment should involve at least an appearance of listening to their opinions; but all these are still seen as add-on, luxury features, subordinate to a general scheme in which doctors must be active and well-informed, but patients may be and usually are passive and ignorant.
Most doctors believe there are big differences in intelligence between patients, that this limits the information patients can accept and recall, and that experienced doctors are able to discriminate between patients who can make good use of discussion of their problems at a reasonably adult level, and those on whom such efforts are wasted.
There is some evidence on how these beliefs work out in practice. Joyce and co-workers (Joyce, C.R.B., Caple, G., Mason, M., Reynolds, E., Mathews, J.A., ‘Quantitative study of doctor-patient communication’, Quarterly Journal of Medicine 1969; ns 38:183-94.) studied 54 patients attending a hospital clinic for rheumatoid arthritis and similar disorders, complaints for which communication (listening and explaining) are often the main help available. Among other things, the doctors rated the patients as more or less articulate. They found that patients rated as more articulate were told more about their condition, and told it more often, than those rated as less articulate, though the proportion of information they retained and understood was the same. In other words, the doctors thought they could identify the better learners, and then gave them more information, though logically one would imagine that slow learners need more rather than less teaching time; retention of the information was not better in those rated by the doctors as more articulate. All doctors I have discussed this with agree that all of us at least initially had this attitude; we may have learned it from schoolteachers, who also traditionally give most attention to their aptest pupils, also believe they can predict learning capacity, and are also frequently proved wrong by rapid progress in many pupils once they have left school.
Similarly, doctors tend to think they can predict compliance. They are wrong; studies have shown that apart from extremes of age, no sociodemographic variables are consistently associated with either compliance or non-compliance. (Menard, J., Degoulet, P., Hong, A.V. et al., ‘Compliance in hyper tension care’. In, Mild hypertension: recent advances, ed. Gross, F.,Strasser, T., p. 349. New York: Raven Press, 1983.), (Haynes, R.B., ‘A critical review of the determinants of patient compliance with therapeutic regimens’. In Compliance with therapeutic regimens, ed. Sackett, D.L., Haynes, R.B., p. 26. Baltimore: Johns Hopkins University Press, 1977.) Doctors are poor predictors of patient behaviour. French physicians who tried to predict who would continue and who would lapse treatment with digitalis and diuretic tablets for heart failure were wrong in 50% of cases, suggesting that their forecasts were no better than random choices(Mushlin, A.I., Appel, F.A., ‘Diagnosing patient non-compliance’, Archives of Internal Medicine 1977; 137:318.).
Are Doctors Interested in what Patients know and think?
Influenced particularly by Balint’s modification of the Osier paradigm, which appears to emphasize patients’ own perceptions of their problems, progressive GPs since the 1970s have been confident that they are moving rapidly towards a more shared, less unequal relationship with their patients, both in defining medical problems and in devising solutions, which should ensure at least an informal level of accountability to patients which might be more effective than a formal structure.
Careful work by David Tuckett (Tuckett, D., Boulton, M., Olson, C., Williams, A., Meetings between experts: an approach to sharing ideas in medical consultations, London: Tavistock Publications, 1985.) and his group has shown conclusively that this is not so. Little if any change has in fact taken place in the overt behaviour of doctors, whether or not they believe such a change to be desirable. Their aim was to explore the extent to which ideas can be shared in medical consultations, because of general agreement by progressive GPs that giving information is often the only available help in a consultation; because patients need information to follow advice and assist them in making difficult choices; because many patients already act as experts in their own self-care (e.g. people with diabetes, asthma, epilepsy, multiple sclerosis) and more should do so; and because patients should be regarded as individuals who interpret and try to make sense of what happens to them.
Their study material was 1,302 tape-recorded consultations by two groups of GPs. The first was a study group of eight, selected because they were recognized trainers responsible for teaching consultation skills, who had attended lengthy RCGP courses in the Balint tradition, deliberately aimed at changing doctors’ behaviour. Some of these GPs had conducted and published research and others had senior university teaching appointments. The comparison group consisted of another eight GPs chosen randomly from lists of NHS GPs in the same areas as the study group. Very detailed studies were made of a random sample of 69 consultations, and of another 405 consultations selected because they included problems likely to require sharing of information.
Their original intention was to look at expected differences in the way these two groups of GPs (one theoretically convinced of the need for mutually shared information, the other with traditional ideas of active doctors and passive patients) actually behaved. In fact there were virtually no differences. All the doctors in both groups appeared in practice to see transmission of information and ideas as an almost entirely one-way process, and none of them sought patients’ ideas about how their problems were caused or defined, or how they might be remedied.
This uniformity of behaviour, despite real differences in attitude and intention which have seriously divided GPs for many years, suggests that virtually all doctors are in fact working within constraints of which they are as yet scarcely conscious (the Osier paradigm). Patients, however assertive they may normally be, also accept these constraints within consultation, so that their own information and intelligence is not used.
Many people will regard this as a rather trivial discovery, hardly warranting the £250,000 of Health Education Council money it consumed. It has long been fashionable to attribute most problems in medical care to the arrogance of doctors and their refusal to share power with the public they serve, in fact this is a central point of the Liberal Critique. Tuckett’s group agrees, but modifies this in critically important ways which make it constructive and helpful rather than divisive and defeatist in its effect:
The pattern of consultation we have observed. . . may, in part, be the product of more or less conscious attempts to maintain hierarchical relationships. But these in turn may result from still more fundamental causes. Virtually all of the doctors whom we studied and with whom we later worked gave us the impression that they were very devoted to the welfare of their patients. In recent years medical practitioners, especially in the UK, have devoted an enormous amount of time and effort to self-evaluation and self-criticism. Many doctors also spend a great deal of time voluntarily trying to improve their skills. . . The need to maintain or create hierarchical relationships can. be caused by other factors than the pursuit of power. For example, the innate conflicts and anxieties built into being a doctor may all too easily produce the need to stay in control. The doctor’s consulting role carries special responsibilities and anxieties and is inherently difficult. He must deal on a day-to-day basis with his own and his patients’ uncertainties, experiences of disaster, failures, helplessness, blame, panic and anxieties, as well as with the unconscious feelings that go with them. Actions must sometimes be taken quickly and routinely without adequate knowledge and with the awareness that a mistake can be fatal. Inevitably decisions will sometimes be hard to justify in cooler moments. The role also involves conflicts arising from social reality: for example, the doctor must mediate the demands of different patients, allocate scarce resources, mediate between the patient and his family and social network, mediate between the needs of his patients and those of himself, etc. To cope with the role both institutional and personal methods of coping have been developed: including, perhaps, tunnel vision, emotional withdrawal, being busy, being obsessed with one or more technical aspects of medicine and being omnipotent in his behaviour. The Apostolic Function [Balint’s term for the effect on an illness of the doctor’s own personality] is a similar defence.
All these fundamental reasons applied even more in the past, when so much of medical care was hopeful illusion, maintained by patient and doctor who colluded in production not of effective care, but of often wilfully blind optimism and evasion of reality. All this has been a part of the Osier paradigm, escape from which requires understanding, not acts of will. Doctors still have to shoulder a great deal of threatening uncertainty, which few experienced people, either doctors or patients, would suggest can at all times be borne equally by both sides; it is still a necessary part of the job for most doctors most of the time to reserve to themselves a burden of uncertainty in diagnosis and prognosis, sharing this with the patient only after a narrower and more tolerable range of possibilities has been defined; otherwise they will add even more to the patient’s own load of uncertainty and fear. Doctors are socially useful workers, a point sometimes overlooked by some of their academic critics.
Are Patients Consumers or Producers’?
Patients, and where there is a freely available health service, the public at large, are often referred to as consumers of medical care. Even the groups which are most hostile to medical dominance generally see the remedy for this in a strengthening of the rights and power of consumers, and see themselves as part of a national or even international consumers’ movement. Doctors chastened by the Liberal Critique are eager to concede this; they see limitation of the hitherto unchallenged authority of doctors as care-providers, and extension of the choices open to patients as consumers, as entirely progressive steps. The idea originated naturally from the private consultation as an essentially commercial transaction, in which doctors created a commodity which patients bought to consume for their personal benefit. Where no commercial transaction took place, for example when Sir William Osier examined a poor patient with an interesting disease at Johns Hopkins or the Radcliffe Infirmary, or later a National Health Service patient was treated free by her GP (what we might call ‘public’ rather than ‘private’ consultations), the rights and powers of patients were diminished and the authority of the doctors increased, because both rested on the unenforceable customs of charity rather than the clearly defined property rights of sale. Beggars can’t be choosers, and accountability in a charity service arises only in extreme cases of breakdown. Patients’ rights appeared to be maximized when they were paying consumers within an essentially commercial transaction.
The Osier paradigm was most apt where patients paid for their care, and were able to choose their doctor and insist on treatment of a quality consistent with its price. Private practice set the optimal level of quality with which State Charity was supposed to stand comparison, and was supposed to be what everyone would want if they could afford it. For doctors influenced by the Liberal Critique this was a slightly uncomfortable conclusion, because they knew very well that marketed medicine is no more trustworthy than marketed motor cars or any other commodity. Caveat emptor, above all when the seller seems to know everything and the buyer almost nothing. Sed quoque caveat vendor; a commercial sale may present a threat to the integrity of the seller as much as to the pocket of the buyer. The relation between all vendors and consumers is inherently adversarial, and liberal doctors remain fundamentally uncomfortable with the consumer-provider relationship.
However, we have seen that medical problems can only be realistically defined by a joint effort between at least two kinds of skilled people: patients skilled in observing their own past history, present symptoms and the social settings within which problems arise and must be solved; and doctors (or other health workers) skilled in interpretation of this information, and able to construct from it a set of realistic diagnostic and therapeutic options. We have also seen that once medical problems are appropriately defined, there cannot be a realistic plan for their containment or solution without the same kind of joint effort, from doctors (or other health workers) who know what kinds of solutions to look for, and from patients who know how they might be applied within the constraints of their real personal lives.
This is a production process, in which various consumptions (tablets, x-rays, doctors’ and patients’ time, etc.) may be necessary, but in which something new is present at the end of a consultation which did not exist at the beginning; a defined set of problems, together with tentative plans for their solution. This view is bad for medical sales. If doctors are to sell their skills as a commodity at the best price, they must discount or even conceal (first of all from themselves) skills contributed by the purchaser. If patients are customers they must be encouraged to think they can buy better health from doctors as a package, but may therefore be less willing to accept that they are going to have to do most of the work. Why buy a dog and bark yourself?
Commercial transactions have almost vanished from British general practice since 1948, yet this conception of patients as consumers not only survives, but is gaining influence. How can this be explained? The idea has certainly gained new strength from the rapid growth of private medical care as the NHS has become less and less able to bridge the gap between public demand and State supply, though little of this has as yet occurred at GP level. It has also been reinforced by the strength of the consumerist movement in general, which, starting in the USA in the 1960s, has provided a popular platform for superficially radical and democratic ideas, without challenging (in fact powerfully reinforcing) the fundamental requirements of capitalism: private investment for the market rather than public investment for human needs, and denial in practice of all creativity which cannot be expressed in commodity terms.
The weakness of this view becomes obvious as soon as we look at the real medical problems of real people. Who was responsible for maintaining the health of Hopkin Morgan? I was, he was, and so were a lot of other people who helped me (orthopaedic surgeons, renal physicians, radiologists and radiographers, laboratory technicians, nurses, etc.) and him (his wife, sons, daughters, mates at work and drinking companions). We were not always successful, and all of us may sometimes have counter-produced; but his present state of health is a social product of work done well or badly by many people, but usually starting from GP and patient in joint consultation. This process can be commercialized, albeit with difficulty. It is possible to break it down to make some of the more suitable fragments into commodities for sale, but not without damage; a jointly produced value which might have been shared and developed further must be divided into a sold profit for the vendor and a bought possession for the consumer, who then owe one another nothing. The episode of diagnosis and treatment becomes isolated, transient and superficial. The transaction damages and limits the value it claims to sell.
All aspects of medical science are advancing, and inevitably this includes high-technology salvage in medical crises, in which the patient is indeed almost entirely passive and dependent on professional skills. In these primitive conditions, the Osier paradigm works. Such care could easily become a commodity for sale if society were sufficiently de-civilized to allow a market in life and death to operate, a possibility which our leaders of public opinion have now made thinkable. But acute care is not the main line of advance of either medical science or medical practice. Most of its effective techniques are already well understood and for the most part fairly well delivered, and many of the most superficially impressive new techniques don’t work in practice. Though the component techniques of (for example) intensive coronary care are impressive when taken one by one in isolation, careful studies in Australia, USA and Scandinavia of death rates from coronary heart attacks in hospitals offering different levels of technical sophistication show that those offering continuous monitoring, specially trained nursing staff for coronary care and emergency resuscitation, a staff cardiologist, and a cardiac surgical service are no more effective than hospitals without these facilities.(Reznik, R., Ring, I., Fletcher, P., Berry, G., ‘Mortality from myocardial infarction in different types of hospitals’, British Medical Journal 1987; 294:1121-5.), (Bain, C., Siskind, V., Neilson, G., ‘Site of care and survival after myocardial infarction”, Medical Journal of Australia 1981; ii: 185-8.), (Bloom, B.S., Peterson, O.L., ‘End results, cost and productivity of coronary care units’, New England Journal of Medicine 1973; 277:72-8.), (Hofvendahl, S., ‘Influence of treatment in a CCU on prognosis in acute myocardial infarction’, Acta Medico Scandinavica 1971;519s:l-78.). Whatever benefits there may have been from more sophisticated technology since the late 1960s are evidently already available at nearly all hospitals, and special units with their very elaborate and expensive care have not improved outcome. More than half the deaths from coronary heart attacks occur during the first two hours after onset of symptoms, but the average delay between onset and arrival at hospital is at least three hours in most parts of Britain, mostly because of delay by patients in sending for a doctor or ambulance, probably because they don’t want to believe the pain has a potentially lethal cause (the process of denial). By the time most patients get to hospital, many of them might as well be looked after at home if family and nursing support are good. (Christiansen, I., Iversen, K., Skouby, A.P., ‘Benefits obtained by the introduction of coronary care unit: a comparative study’, Acta Medico Scandinavica 1971; 189:285-91.),(Mather, H.G., Pearson, N.G., Read, K.L.Q., et al., ‘Acute myocardial infarction: home and hospital treatment’, British Medical Journal 1976; i:925-9.), (Hill, J.D., Hampton, J.R., Mitchell, J.R.A., ‘A randomized controlled trial of home-vs-hospital management for patients with suspected myocardial infarction’, Lancet 1978; i:837-41.)
Future advance in medical care will only develop on a mass scale through prevention or limitation of organ damage by strategies which depend on changes in human behaviour, or on interventions arising from the revolution in molecular biology which will be prompted by findings from population screening rather than presented symptoms. Much of this could be achieved by improved living conditions for the whole population, better education, full participation in society and better customs of eating, working and playing freed from commercial pressures; but we will also need the precise individual targeting and support which could be available from professional health workers, if they were helped to escape from the Osier paradigm by a socially-oriented NHS which set targets and measured their attainment. Of course we need public health campaigns directed at the whole population, but the real test of useful change is whether we are giving effective help to the most vulnerable groups in immediate danger of irreversible organ damage, people with chronic disorders such as asthma, diabetes, high blood pressure, schizophrenia or epilepsy, and the honest present answer has to be that for the most part we are not. Previous chapters of this book have documented the evidence of incomplete care, with many patients still undiagnosed, and many more who have entered the care system but then dropped out because it is not geared to their needs.
Riddle’s Five Steps for Effective Care of Chronic Disease
In his paper ‘A strategy for chronic disease’, Matthew Riddle (Riddle, M.C., ‘A strategy for chronic disease’, Lancet 1980; ii:734-6.) an American specialist in diabetes, gave a perceptive review both of what’s wrong with medical care now and what needs to be done to put it right. The example he gives concerns diabetes, but applies equally well to every other chronic disorder:
diagnosis and treatment [of diabetes] is not the major problem. . . We first make recommendations concerning diet and physical activity. If plasma glucose remains high, we prescribe oral drugs or insulin. But here begins the larger problem. These interventions must be more or less permanent and demand daily attention by the patient. They may require major changes in behaviour and the pattern of daily life. Thus, they are not treatments in the usual sense, administered by an expert to a passive beneficiary; they are new ways of living. A major and sustained change in behaviour is easy to discuss but hard to achieve. ..
Research presses on at great cost, with substantial yield. . . We have new tools and better models of the old ones: purer insulins, accurate disposable syringes, glucose-oxidase strips, home glucose analysers and, on the way, the first generation of hang-from-the-shoulder, open-loop artificial pancreases.
All these innovations are helping, yet they are not enough. They are, I think, slightly off the target. For one thing, more sophisticated specialists, systems and gadgets will bring more sophisticated forms of disaster. . . But my main concern is that we are juggling the parts without assessing the whole… We need a new strategy.
Management of diabetes is a process which can be divided into five steps. All the steps must be completed if management is to be as satisfactory as possible. They have a logical sequence. Completion of the later steps reinforces the earlier ones, so management improves with time. Each step must be recognized as part of the overall plan, not over-valued for itself.
- Acquisition by the health professionals involved of an adequate base of information about the disorder.
- Acceptance by the patient of primary responsibility for coping with the disorder and maintaining health.
- Learning by the patient of the physiology, complications, and details of treatment.
- Negotiation between patient and health professionals of general goals and specific objectives for management acceptable to both.
- Assessment of success in meeting the objectives using quantitative measures understood by both patient and health professional.
… a systematic approach to chronic disease should become a central part of our medical heritage, together with the scientific method for research and the responsibility of the healer for the acutely ill. This five-part strategy may be a start.
Medical care that is effective and available to all who need it, rather than illusory and promoted on the market or distributed charitably as an appearance of care without verified effect, is a social product in which patients as much as doctors need to become central performers. Escape from the tradition of doctor-centred consultation requires more than the narcissistic self-criticism of Balintry in practice, however patient-centred it may appear in theory.
It requires first of all that doctors insist on having enough time to do their work properly, while also insisting that this quality of service must be available to the whole population as a human right. Effective consultations, which maximize inputs from patients and outputs in relevant action consistently applied, cannot be done within the 5 minute, 5×7 inch format of Lloyd George industrial practice. Unhurried, friendly, thoughtful consultation is not a luxury for the future, but a present necessity for effective care, and it’s time both patients and GPs insisted on having it.
Secondly, doctors and patients must recognize the limited clinical effectiveness of the Osier paradigm, so that they no longer see the doctor-centred, episodic technical fix as the core of good practice, to which patient-centred ideas may be bolted on as an afterthought.
The alternative paradigm is anticipatory care democratized at the design stage to include both active outreach from care-giver to patient, and active responsibility of the patient for definition and solution of problems. The only valid test of its capacity to deliver medical science more effectively than the Osier paradigm will be its effect not on individual cases at anecdotal level, but on the morbidity and mortality of populations, which leads us to the next chapter.
